-
What Is Central Serous Retinopathy (CSR)?
Central Serous Retinopathy, also known as Central Serous Chorioretinopathy, occurs when fluid builds up beneath the retina, causing visual distortion. When fluid accumulates under it, it leads to a detachment of the retina, resulting in blurred or distorted vision. CSR primarily affects the macula—the central part of the retina responsible for sharp, detailed vision. It is more common in men between the ages of 20 and 50, although women and older adults can also experience it.
Causes of Central Serous Retinopathy:
The exact reason for fluid leakage under the retina isn’t always clear, but several factors increase the risk of developing CSR:
• Stress:
High stress levels trigger an overproduction of cortisol; a hormone linked to CSR.
• Corticosteroid Use:
Prolonged use of corticosteroids, whether oral, topical, or injected, is a major risk factor.
• High Blood Pressure:
Hypertension can damage blood vessels in the eye, contributing to fluid buildup.
• Obstructive Sleep Apnoea:
This condition can affect oxygen levels, potentially impacting retinal health.
• Age and Gender:
Men between the ages of 20 and 50 are at a higher risk.
• Genetics:
A family history of CSR increases the likelihood of developing the condition.
Common Symptoms of Central Serous Retinopathy:

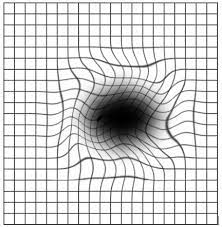
• Blurred Central Vision: Difficulty seeing objects clearly in the centre of your field of vision.
• Gray or Dark Spots: You may notice areas of dim vision or Gray spots.
• Distorted Images:Straight lines may appear wavy or bent (a symptom called metamorphopsia).
• Reduced Contrast Sensitivity:Difficulty distinguishing between similar shades or colors.
• Light Sensitivity:Increased sensitivity to bright light.
• Micropsia:Objects may appear smaller than they actually are.
If you experience any of these symptoms, seek an eye specialist’s advice
What are the Sign & Symptoms ?
If only one eye is affected to begin with, the symptoms may not be noticeable in early stages. Gradually as disease progresses or if both eyes are involved, reading or close work may become difficult. Common symptoms are distortion of objects which are looked at directly, for e.g. bulges or curved appearance of a straight door, distorted print lines in book (metamorphopsiae), missing of letters or words while reading, a dark or blank spot in the center of vision, (scotoma) or fading of colors specially blue (dyschromatopsiae).
How is it Diagnosed ?
As initially it is a silent disease, mostly it is picked up in a routine retina examination by an ophthalmologist .The retinal examination done by an ophthalmoscope will show the findings of this disease process. To assess the condition in detail, certain other test are done:
* Amsler Grid: It is a test paper with graphic picture to be used at reading distance with near glasses on. This is used to check for extent of sight loss-dark spot, distortion or missing of straight lines and also is given to the patient to take home so that he can monitor his symptoms at home and report immediately if there is worsening.
* Fundus Fluorescin Angiography (FFA) / Indocyanine Green Angiography (ICG): the photographs of macula are taken after injecting a dye in patient’s arm. The dye reaching the eye helps to clarify the type and extent of disease, including detail of abnormal vessels, leaks and membrane formations.
* Optical Coherence Tomography (OCT) : In this test photographs of the retina are taken to show its microscopic detail. So it can help detect any early thickening of the retina in wet ARMD. Also it can delineate the abnormal blood vessels ( choroidal neovascularisation ) from where the blood oozes. Changes of dry ARMD such as drusen can also be demonstrated. Also it is an excellent tool to follow up after treatment to assess the effect of the treatment done and need for re-treatment.
Managing and Preventing CSR
Preventing CSR eye disorder involves addressing the underlying risk factors and adopting healthy habits:
• Manage Stress:
Regular physical activity, meditation, and relaxation techniques such as yoga or deep breathing exercises can help reduce stress levels, which is a major trigger for CSR.
• Limit Corticosteroid Use:
Consult your doctor before taking or discontinuing corticosteroids. If you rely on these medications, discuss possible alternatives or dose adjustments.
• Control Blood Pressure:
Maintain a healthy diet rich in potassium (bananas, spinach), magnesium (nuts, seeds), and omega-3 fatty acids (salmon, chia seeds) to support vascular health and reduce blood pressure.
• Eye-Healthy Foods:
Include foods rich in antioxidants, such as berries, oranges, and leafy greens, which help reduce oxidative stress in the eyes. Carrots, known for their high vitamin A content, can also boost overall eye health.
• Routine Eye Exams:
Regular check-ups can catch the condition early and prevent complications. Follow up with your ophthalmologist if you have any recurring symptoms or risk factors.
By integrating these practical measures into your lifestyle, you can manage and potentially prevent the onset or recurrence of CSR.
-
What is Conjunctivitis?
Inflammation of conjunctiva (Transparent membrane covering white part of the eye) is called Conjunctivitis. It is a condition where the eye turns red. Conjunctivitis can be due to bacteria, virus, allergy, etc. List of allergens are endless and individual specific. It causes itching, redness, and watering,discharge from eyes.
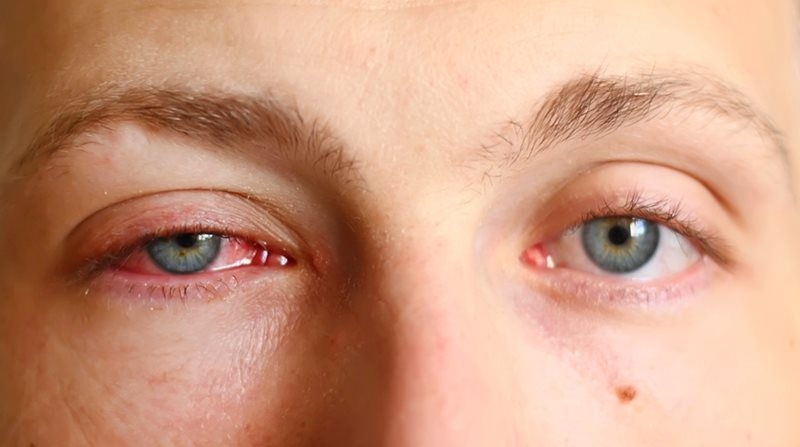 Symptoms and Signs of Conjunctivitis
Symptoms and Signs of Conjunctivitis
Below we have mentioned some of the many signs of allergic conjunctivitis:
• Itching
• Watery eyes
• Redness & swelling
• Foreign body sensation
• Discomfort to light
• Discharge
Causes of Conjunctivitis
• Bacterial
• Viral
• Chemical
• Allergy
List of allergens
• Dust
• Cosmetics (Kajal, eye liners, Mascara etc)
• Air pollution
• Smokes
• Eye drops (used for longer period like Anti glaucoma drops etc.)
-
What is Computer Vision Syndrome?
Computer Vision Syndrome (CVS), also known as digital eye strain, is a condition caused by prolonged use of digital screens, including computers, tablets, and smartphones. Staring at screens for extended periods forces the eyes to continuously focus and refocus, leading to visual fatigue and discomfort. The blue light emitted from screens and the constant glare contribute to screen eye strain, making it difficult for the eyes to remain comfortable. Common computer vision syndrome symptoms include eye fatigue, headaches, blurry vision, dry eyes, and neck pain. If left unmanaged, CVS can significantly impact productivity and overall eye health. Taking preventive measures like adjusting screen brightness, maintaining proper posture, and following the 20-20-20 rule can help reduce digital eye strain symptoms and improve visual comfort.
Symptoms of Computer Vision Syndrome
The symptoms of computer eye syndrome vary from person to person, depending on screen usage and underlying eye conditions. Some of the most common computer vision syndrome symptoms include:
• Eye strain and fatigue:
Constant screen exposure forces the eyes to work harder, leading to tiredness.
• Blurred vision:
Difficulty focusing on the screen or seeing clearly after prolonged use.
• Dry eyes:
Reduced blinking rate causes irritation, redness, and a burning sensation.
• Headaches and neck pain:
Poor posture and screen positioning contribute to musculoskeletal discomfort.
• Sensitivity to light:
Prolonged exposure to bright screens can increase light sensitivity. Recognizing these digital eye strain symptoms early can help prevent severe vision discomfort and long-term complications
Causes of Computer Vision Syndrome
Several factors contribute to the development of computer eye syndrome:
• Prolonged screen exposure:
Extended screen time forces the eyes to continuously focus, causing fatigue.
• Glare and blue light:
Digital devices emit harmful blue light, which can lead to screen eye strain and disrupt sleep patterns.
• Poor posture and viewing distance:
Sitting too close or too far from the screen increases strain on the eyes and neck muscles.
• Infrequent blinking:
People blink less frequently when using screens, leading to dry eyes and irritation.
• Uncorrected vision problems:
Individuals with refractive errors (nearsightedness, farsightedness, astigmatism) may experience worsened digital eye strain symptoms if their prescription glasses are outdated.
Risk Factors for Computer Vision Syndrome
• Certain factors increase the likelihood of developing digital eye strain:
• Excessive screen time:
Individuals who spend more than 6 hours daily on digital devices are at higher risk.
• Improper lighting:
Working in poorly lit environments or excessive glare worsens symptoms.
• Age:
Older adults and individuals with existing eye conditions experience more discomfort.
• Work-related exposure:
Professionals in fields requiring prolonged screen use, such as IT workers, designers, and students, are at higher risk.
• Lack of screen breaks:
Not following the 20-20-20 rule (looking away from the screen every 20 minutes for 20 seconds at an object 20 feet away) increases eye strain. Reducing screen exposure, optimizing lighting conditions, and wearing blue-light-blocking glasses can help minimize computer eye syndrome symptoms.

Home Remedies and Lifestyle Changes to Reduce CVS
• To reduce computer eye syndrome symptoms, incorporate these home remedies:
• Follow the 20-20-20 rule:
Take breaks to rest eye muscles.
• Blink frequently:
Consciously increase blinking to prevent dry eyes.
• Use anti-glare screen protectors:
These minimize screen glare, reducing digital eye strain symptoms.
• Adjust screen brightness and contrast:
Optimize display settings to reduce eye fatigue.
• Stay hydrated:
Proper hydration supports tear production and prevents dry eyes.
These simple changes can effectively minimize computer vision syndrome symptoms.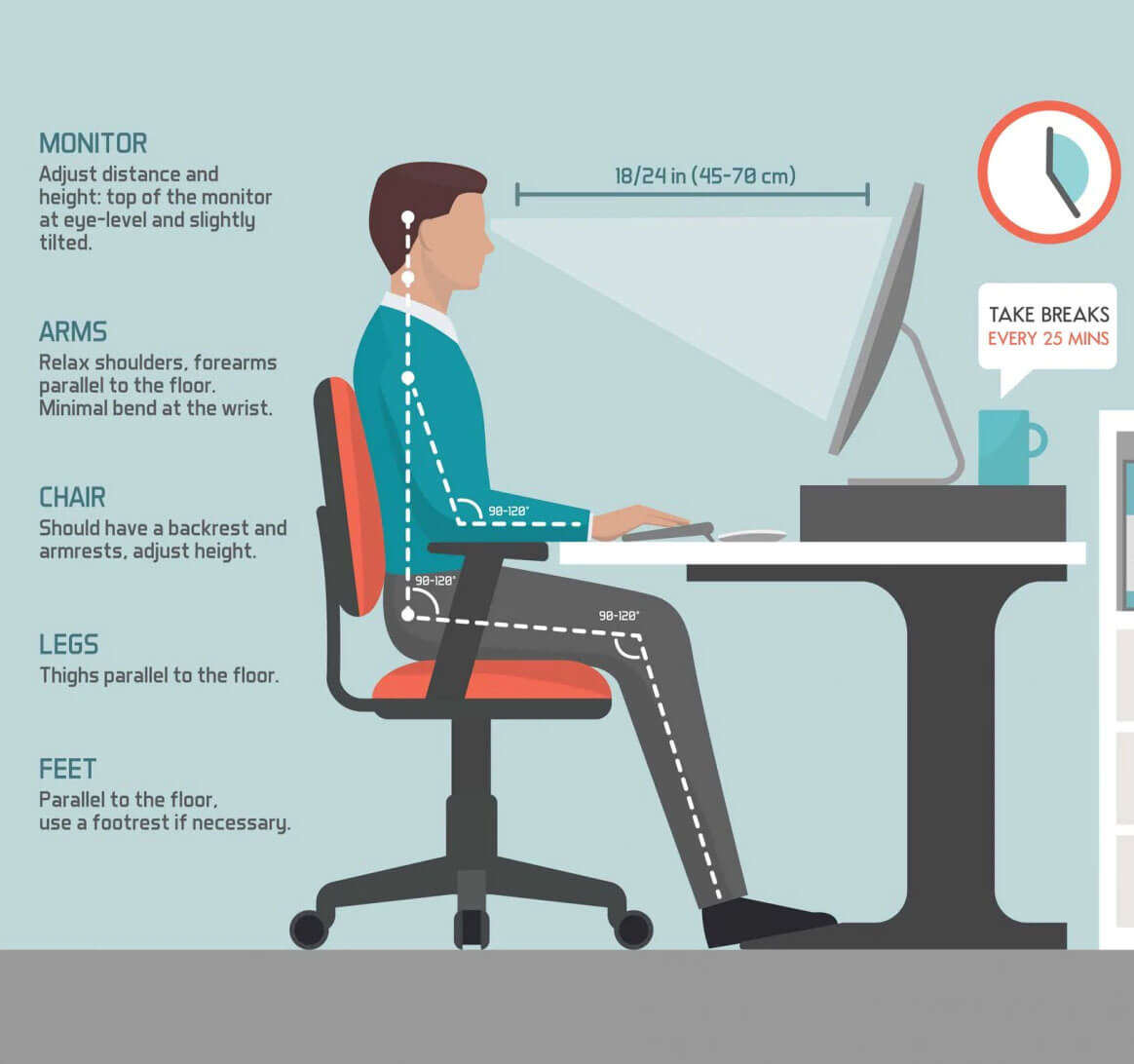 Eye Exercises to Prevent Computer Vision Syndrome
Eye Exercises to Prevent Computer Vision Syndrome
• Incorporating eye exercises can help relieve digital eye strain symptoms:
• Blinking exercises:
Close and open eyes slowly to restore moisture.
• Focus shifting:
Alternating focus between near and far objects relaxes eye muscles.
• Palming technique:
Rubbing hands together and placing them over closed eyes can relieve stress.
• Eye rolling:
Gently rolling the eyes helps improve circulation and reduce stiffness.
Practicing these simple exercises daily can enhance eye comfort and prevent screen eye strain.
-
What is cataract?
Symptoms & Treatment:
An eye cataract forms when the lens of the eye becomes cloudy, making it harder to see clearly. The lens, which is normally clear, helps focus light on the retina to produce sharp vision. When it becomes cloudy, it can cause cataract symptoms like blurry vision, glare, and trouble with night driving. Although common in older adults, eye cataracts can also be caused by injuries, medical conditions, or prolonged UV exposure.
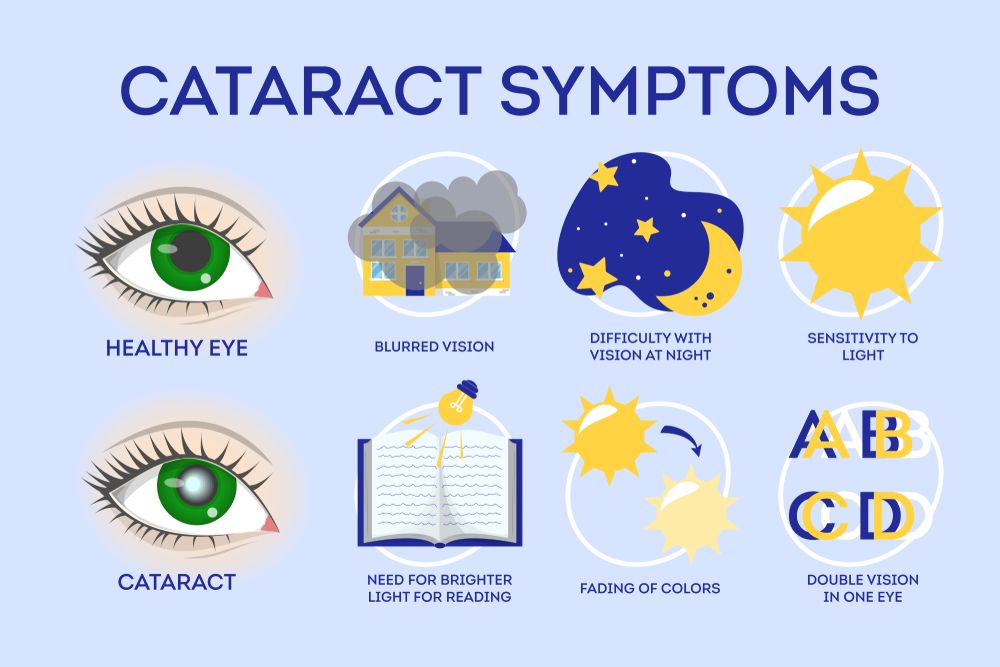
Most Common Cataract Symptoms Include:
Cataract symptoms vary depending on the type and stage of the cataract. Common cataract signs and symptoms in the eye include:
• Cloudy or Blurred Vision: Objects may appear fuzzy, and vision may feel foggy or unclear.
• Sensitivity to Light and Glare: Bright sunlight, headlights, or even indoor lighting can cause discomfort and difficulty seeing.
• Poor Night Vision: Difficulty seeing in low light or during night time activities, such as driving, is common.
• Fading or Yellowed Colors: Colors may lose their vibrancy, appearing dull or washed out.
• Halos Around Lights: Seeing halos or rings around bright lights, especially at night.
• Double Vision in One Eye: Some patients report seeing double images due to the clouded lens.

What are the Causes of Cataract?
There are several causes of cataract, with aging being the most common. Other factors that lead to the formation of cataracts include:
• Aging: Natural changes in the lens cause protein breakdown and cloudiness, resulting in cataracts.
• Eye Injuries: Trauma to the eye can lead to cataract formation, either immediately or years later.
• Family History: A family history of cataracts increases the risk.
• Medical Conditions: Conditions like diabetes significantly increase the likelihood of developing cataracts.
• UV Exposure: Prolonged exposure to ultraviolet rays without proper eye protection can damage the lens.
• Steroid Use: Long-term use of corticosteroids can accelerate cataract formation.
• Smoking and Alcohol: Both habits contribute to oxidative damage in the eye and increase the risk of cataracts.
How to Prevent Eye Cataract?
While not all cases of cataracts can be prevented, adopting healthy habits can help delay their onset. Here’s how you can reduce your risk of developing eye cataract symptoms:
• Wear UV-Protective Sunglasses: Protect your eyes from the harmful effects of ultraviolet light.
• Maintain a Balanced Diet: Include antioxidant-rich foods like leafy greens, carrots, and citrus fruits in your meals.
• Quit Smoking: Smoking damages eye tissues and contributes to cataract formation.
• Control Medical Conditions: Proper management of diabetes and other health issues can reduce the risk of cataracts.
• Limit Alcohol Consumption: Reducing alcohol intake helps protect overall eye health.
• Regular Eye Check-Ups: Routine eye exams allow for early detection and management of cataracts.
Treatment of cataract
Cataract surgery Cataract if left untreated, it can lead to blindness.Luckily, this blindness causing eye disease is reversible. At the right stage your eye doctor will advise and perform Cataract surgery.
What happens in cataract surgery?
In the cataract treatment procedure, eye care specialists numb the area around your eyes with local anaesthesia before the cataract eye surgery, but you are awake throughout. Under this cataract operation, eye surgeons remove the clouded lens using a microsurgical instrument and replace it with an artificial intraocular lens (IOL). The entire process and the cataract surgery take less than 20-30 minutes. This means no need of night stay at the hospital.
Post-Surgery Care Tips
During the cataract operation, patients feel little to no pain. To recover faster after a cataract operation, here are some tips:
• After a cataract operation, you may feel some irritation in your eyes. It is essential to shield your eyes with eyeglasses and avoid dirt or dust affecting your eyes after cataract treatment.
• Do not perform activities like heavy weightlifting to avoid additional eye pressure after cataract removal surgery.
• After a cataract operation, you may see things brighter, so it is essential to avoid driving.
• Take the necessary precautions your doctor suggests and take medications as a cataract cure promptly.
Eyeglasses After Cataract Surgery
Patients, who are comfortable with the idea of wearing spectacles after their cataract operation, can choose monofocal lens. These types of artificial lenses have one focal point as the name suggests. However, now with all the latest advancements it is possible to have minimum dependence on glasses after the cataract surgery. Multifocal or trifocal lenses can go a long way in reducing the dependence on the glasses. It is a good idea to discuss the options of these advanced IOL’s with your cataract surgeon and explore your suitability for them. There are some times when you have minor eye power after cataract surgery; you may need to wear eyeglasses.
-
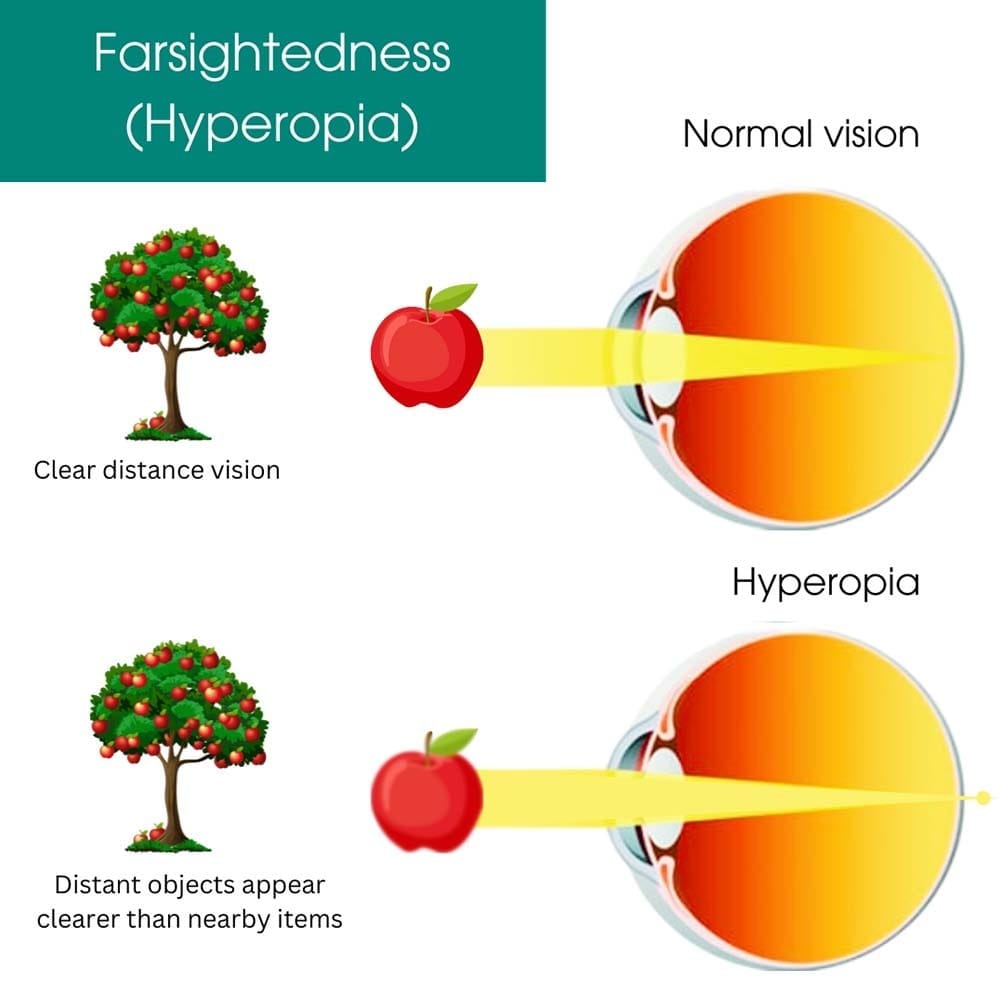
What is Hyperopia?
Hyperopia is a common refractive error where distant objects are seen more clearly than objects close by. If you’re reading a menu at a restaurant and the words appear fuzzy or hard to decipher, you may be experiencing the effects of farsightedness. This condition occurs when the eyeball is too short or when the cornea (the outer covering of the eye) is not curved enough to focus light properly on the retina. In a normal eye, light focuses directly on the retina—the part of the eye responsible for converting light into signals for the brain to interpret as images. However, in someone with hyperopia, light focuses behind the retina, making nearby objects appear blurry. Hyperopia is not only inconvenient but can also cause significant discomfort over time if left untreated. For children, it can affect academic performance, while adults may find it disrupts daily activities like reading or working on a computer.
Causes of Hyperopia: What’s Behind Farsightedness?
Understanding the causes of hyperopia is the first step toward addressing it. The following are some common factors that lead to the condition:
• Genetics:
If one or both of your parents are farsighted, there’s a high chance you could be too. Genetic predisposition plays a significant role in how your eyes develop.
• Eye Structure:
In many cases, hyperopia results from an eyeball that is shorter than normal. This structural abnormality prevents light from properly focusing on the retina.
• Corneal Issues:
A flatter or less curved cornea can affect how light enters the eye, leading to hyperopia.
• Age:
Although hyperopia can affect people of all ages, age-related changes in the lens’s flexibility can exacerbate the condition, especially after the age of 40.
• Underlying Health Conditions:
Certain conditions, such as diabetes or conditions affecting the eye’s anatomy, may contribute to hyperopia.
Signs and Symptoms

Not all cases of hyperopia are obvious. Sometimes, it can develop gradually, making it harder to spot early on. Here are the key symptoms to watch for:
• Blurred Vision:Difficulty focusing on nearby objects like books, mobile devices, or computer screens.
• Eye Strain:Frequent squinting, rubbing of the eyes, or experiencing fatigue after tasks requiring near vision.
• Headaches:Persistent headaches after reading or screen use.
• Difficulty Reading:Small print appears blurry or requires holding materials farther away to see clearly.
• Lazy Eye (in children):If untreated, hyperopia in children can lead to amblyopia or strabismus, where the eyes do not align properly.
Treatment Options: Correcting Your Vision
 The good news is that hyperopia can be easily managed through various treatments designed to correct the refractive error and provide clear vision.
1. Eyeglasses
Eyeglasses are the simplest and most common solution for hyperopia. With the right prescription, they can correct the way light enters your eyes, allowing you to see close objects clearly. Plus, glasses come with the added benefit of being stylish and easy to maintain.
2. Contact Lenses
For those who prefer an alternative to glasses, contact lenses are a popular option. They sit directly on the eye’s surface and provide a wider field of vision compared to glasses. However, they do require proper cleaning and maintenance.
3. Refractive Surgery (LASIK, SMILE, and More)
For a more permanent solution, surgical options such as LASIK or SMILE (Small Incision Lenticule Extraction) are highly effective. These procedures reshape the cornea to correct how light is focused on the retina, offering long-term relief from hyperopia. Dr Agarwals Eye Hospital is at the forefront of advanced refractive surgeries, providing safe and effective options tailored to your needs.
4. Orthokeratology (Ortho-K)
This non-surgical option involves wearing specially designed contact lenses overnight to reshape the cornea temporarily. It’s an excellent option for those seeking freedom from daytime glasses or lenses.
Hyperopia in Children: Why Early Detection Is Crucial
The good news is that hyperopia can be easily managed through various treatments designed to correct the refractive error and provide clear vision.
1. Eyeglasses
Eyeglasses are the simplest and most common solution for hyperopia. With the right prescription, they can correct the way light enters your eyes, allowing you to see close objects clearly. Plus, glasses come with the added benefit of being stylish and easy to maintain.
2. Contact Lenses
For those who prefer an alternative to glasses, contact lenses are a popular option. They sit directly on the eye’s surface and provide a wider field of vision compared to glasses. However, they do require proper cleaning and maintenance.
3. Refractive Surgery (LASIK, SMILE, and More)
For a more permanent solution, surgical options such as LASIK or SMILE (Small Incision Lenticule Extraction) are highly effective. These procedures reshape the cornea to correct how light is focused on the retina, offering long-term relief from hyperopia. Dr Agarwals Eye Hospital is at the forefront of advanced refractive surgeries, providing safe and effective options tailored to your needs.
4. Orthokeratology (Ortho-K)
This non-surgical option involves wearing specially designed contact lenses overnight to reshape the cornea temporarily. It’s an excellent option for those seeking freedom from daytime glasses or lenses.
Hyperopia in Children: Why Early Detection Is Crucial
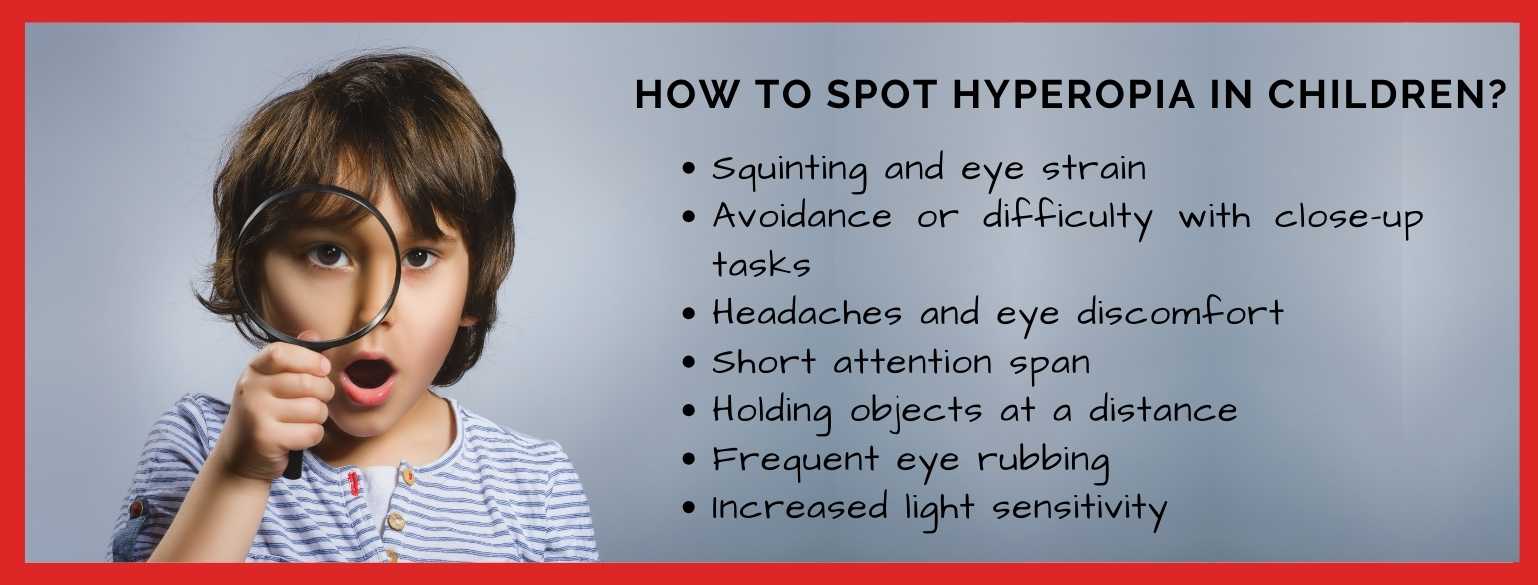
• Children are often unaware of their vision problems, making it essential for parents to ensure regular eye check-ups. Untreated hyperopia in children can lead to developmental delays, difficulty in school, and other complications like lazy eye. Signs that your child may have hyperopia include difficulty concentrating in class, holding books too far from their face, or complaints about headaches and fatigue. Early diagnosis ensures effective treatment and prevents long-term issues. Managing Hyperopia: Tips for Eye Health
• While treatment options are essential, there are also lifestyle changes and habits you can adopt to maintain overall eye health and manage symptoms effectively:
• Follow the 20-20-20 Rule:Every 20 minutes, look at something 20 feet away for 20 seconds to reduce eye strain.
• Limit Screen Time:Excessive screen time can strain your eyes and worsen hyperopia symptoms.
• Eat a Balanced Diet:Foods rich in vitamins A, C, and E, along with omega-3 fatty acids, are beneficial for eye health.
• Regular Eye Exams:Periodic check-ups ensure that any changes in vision are addressed promptly.
-
What is Hypertensive Retinopathy?
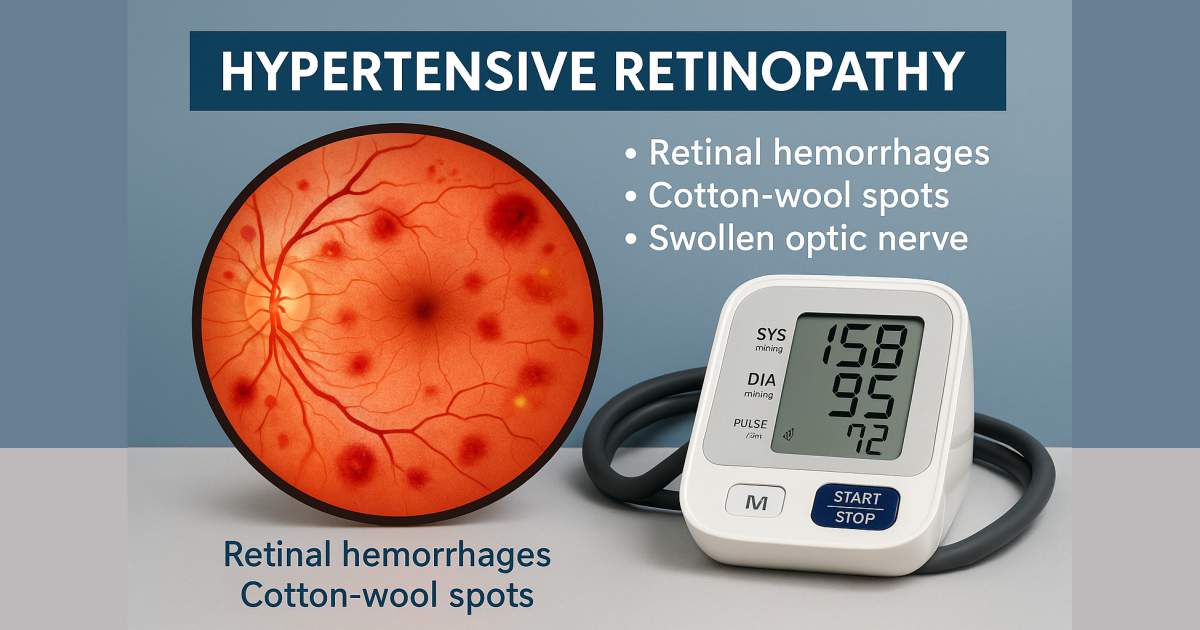
It is damage to the retina and the retinal circulation (Blood vessels) due to systemic hypertension (i.e. high blood pressure). Patients with hypertensive Retinopathy will present with virtually no visual symptoms till profound vision loss. They usually report with headaches or blurred vision. Hypertension can also damage the choroidal circulation and is responsible for optic and cranial neuropathies. Hypertension may also present in the form of subconjunctival haemorrhages.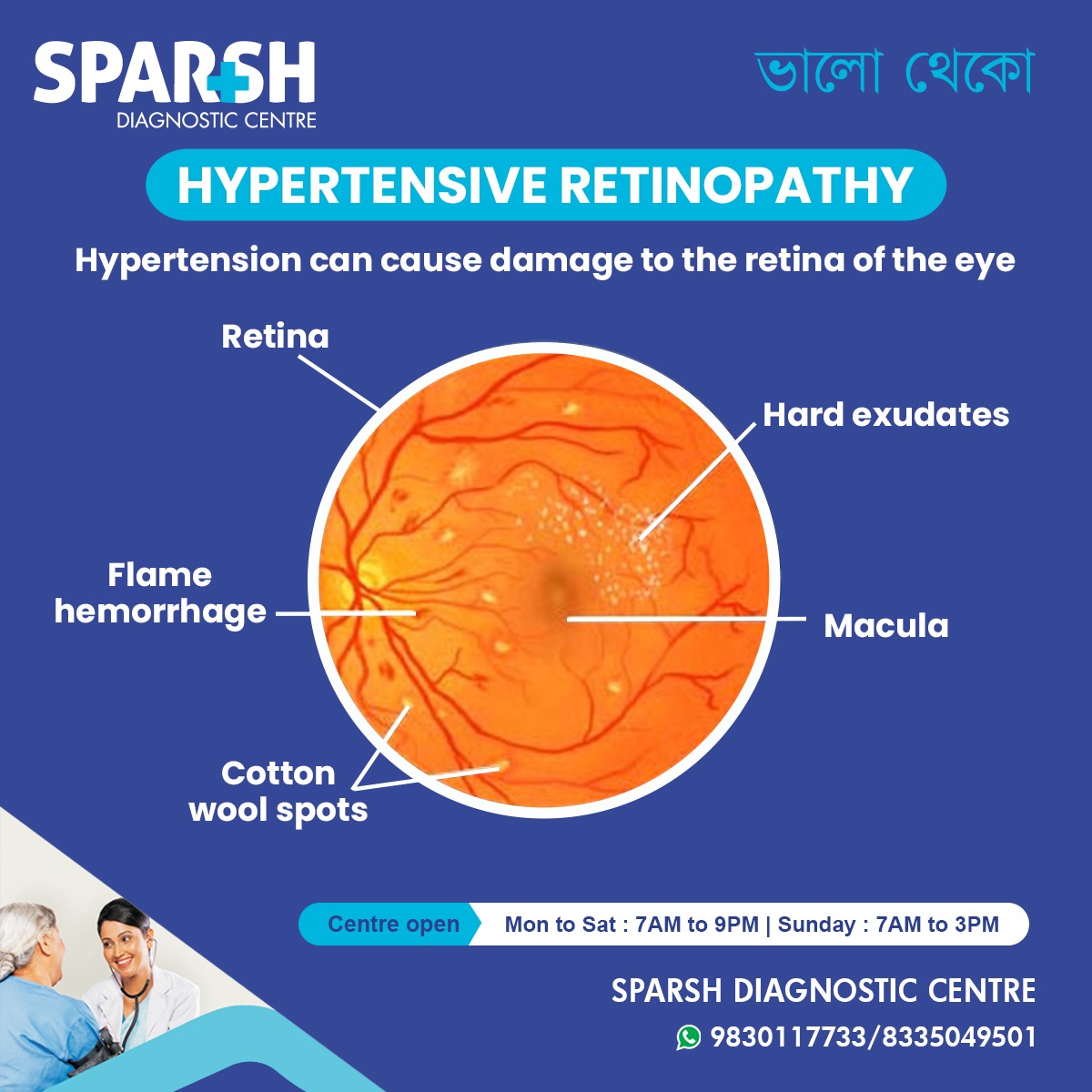
How Hypertension affects the eyes?
Systemic Hypertension is defined as a systolic pressure greater than 140 mm Hg or diastolic pressure greater than 90 mm Hg. Most ocular abnormalities are associated with systolic blood pressures greater than 160 mm Hg. Hypertension affects all organs in the body where small blood vessels are there, like Retina and Kidney.
Smaller blood vessels bear the most brunt of raised blood pressure. The diffuse arteriolar narrowing is characteristic of hypertensive Retinopathy, this is secondary to vascular constriction in acute Hypertension and due to raised cholesterol in chronic Hypertension.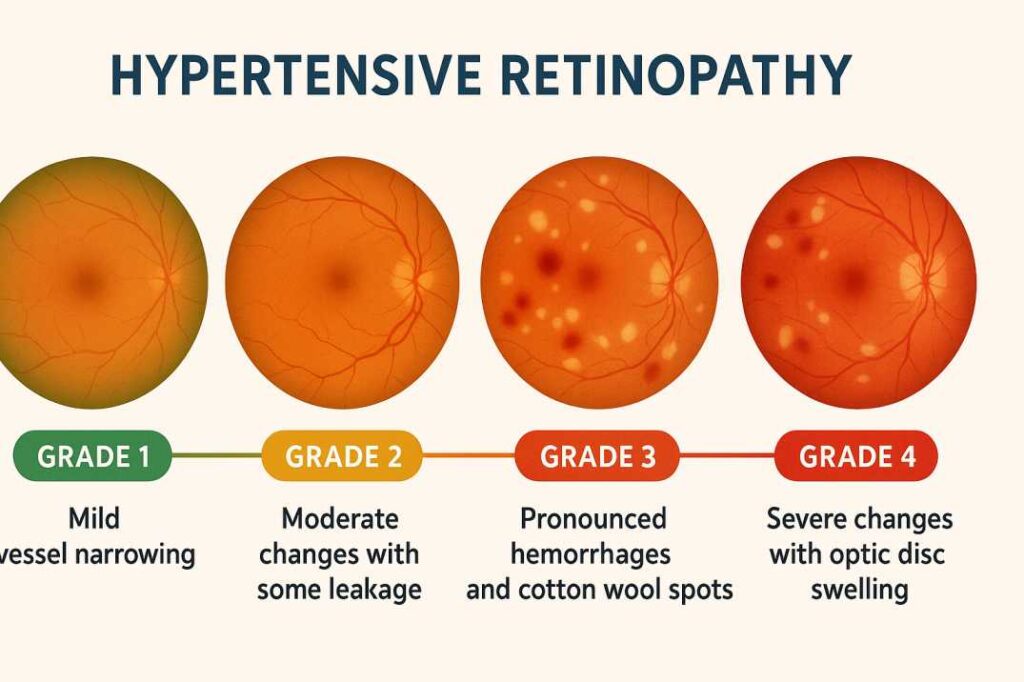
Hypertensive Retinopathy Complications
Patients of hypertensive Retinopathy are vulnerable to several health-related complications like:
• Retinal artery occlusion: This takes place when an artery in the retina of the eye gets closed or blocked due to clots that often result in vision loss.
• Malignant Hypertension: This leads to a rapid spike in blood pressure which can cause vision loss. However, this is a rare occurrence that, in many cases, can be life-threatening.
• Retinal vein occlusion: This condition takes place when a vein in the retina gets blocked because of clots.
• Ischemic optic neuropathy: In this scenario, the normal blood flow that goes to the eye gets blocked, which damages the optic nerve of the eye. It is this part that transmits multiple images to the brain.

Management of Hypertensive Retinopathy
In hypertensive Retinopathy, it is imperative to understand that the only way to treat or control it is by keeping high blood pressure in check. This can be achieved by bringing drastic changes in daily lifestyles like:
• Practising yoga and regular exercise
• Quitting habits like smoking and reducing alcohol intake
• Losing weight and bringing dietary changes.
As mentioned above, symptoms of hypertensive retinopathy stages can be controlled by bringing healthy and positive life changes. In addition, if you want to take allopathy treatment, it is best to get in touch with a doctor who might suggest medications like calcium channel blockers, beta-blockers, angiotensin-2 receptor blockers (ARBs), ACE inhibitors, thiazide diuretics, and more to lower your high blood pressure levels.
-
What is Corneal Ulcer (Keratitis)?
A corneal ulcer (keratitis) is an erosion or an open sore on the cornea which is the thin clear structure of the eye that refracts light. If the cornea becomes inflamed due to infection or injury, an ulcer may develop.
Symptoms of Corneal Ulcer (Keratitis)
• Redness
• Pain
• Watering
• Gritty sensation
• Blurry vision
• Discharge
• Burning
• Itching
• Light sensitivity
Causes of Corneal Ulcer (Keratitis)
• Contact lenses –
contaminated solution, poor hygiene, over usage, sleeping with contact lenses on, using tap water or swimming with contact lens on. Wearing lenses for extended periods blocks the supply of oxygen to the cornea, making it susceptible to infections.
• Trauma –
chemical injury, thermal burn, bee sting, animal tail, makeup or vegetative matter like the branch of a tree, sugarcane.
• Post-surgery –
delayed healing, loose sutures
• Lid deformities –
inward or outward turning of eyelid, misdirection of eyelashes constantly rubbing over the cornea, incomplete closure of eyes
• Decreased nerve supply to the cornea –
seen in diabetics and bell’s palsy patients
• Allergic conjunctivitis
• Vitamin A deficiency
• Prolonged use of eye drops –corticosteroids
• Severe dry eyes –
caused by medical conditions like diabetes mellitus, thyroid disorder, vitamin A deficiency, rheumatoid arthritis, Sjogren syndrome, Stevens-Johnson syndrome
Risk factors of corneal ulcer (keratitis)
• Injury or chemical burns
• Eyelid disorders that prevent proper functioning of the eyelid
• Dry eyes
• Contact lens wearers
• people who have or have had cold sores, chicken pox or shingles
• Abuse of steroid eye drops
• Diabetics
Corneal Ulcer (Keratitis) Prevention
• Do not sleep with contact lenses.
• Do not overuse contact lenses.
• Wash your hands before putting the lenses.
• Advised to use daily disposable lenses.
• Do not use tap water as lens solution.
• While riding a bike, wear eye protection or visor to prevent foreign bodies from entering the eye.
• Do not rub your eye.
• Proper instillation of eyedrops. The nozzle of the eye drop bottle should not touch the eye or the finger.
• Use artificial tears in case of dry eyes.
• Wear protective eyewear when working with wood or metals, especially when using a grinding wheel, hammering on metal, or welding.
• Do not use over-the-counter eye drops.
- What is Blepharitis (Eyelid Inflammation)?
• Blepharitis is a common and chronic condition that causes inflammation of the eyelids. It can affect people of all ages and is often associated with underlying skin conditions or bacterial infections. The condition leads to irritation, redness, and discomfort along the edges of the eyelids. Symptoms of Blepharitis (Eyelid Inflammation)
• The symptoms of blepharitis vary depending on the type and severity of the condition. Common symptoms include:
• Burning sensation, Itching, and Scaling of Eyelids
Patients often experience persistent irritation, leading to an itchy and burning sensation. The buildup of debris on the eyelids may cause crusty eyelids, leading to discomfort.
• Crusty Eyelids
Crusting along the lash line is a hallmark symptom of blepharitis. This can cause discomfort, particularly upon waking up. In cases of squamous blepharitis, flaky skin along the eyelids is commonly observed.
• Photophobia, Blurred Vision, and Foreign Body Sensation
Severe cases of blepharitis can lead to light sensitivity (photophobia) and blurred vision due to tear film instability. The sensation of having a foreign body in the eye is another common complaint among patients.
• Watering of Eyes
Excessive tearing or epiphora may occur as the eye tries to counteract dryness and irritation caused by inflammation.
• Red Eye
The inflammation associated with blepharitis often causes redness, making the eyes appear irritated. Causes of blepharitis can include bacterial infections, skin conditions like rosacea, or mite infestations such as demodex blepharitis.
• Loss of Eyelashes
Chronic blepharitis can lead to lash misalignment, thinning, or even loss of eyelashes, medically termed madarosis. Blepharitis medication may be required to prevent complications.
• Recurrent Stye
People with blepharitis are at a higher risk of developing styes—painful, red lumps along the eyelid margin. Some cases of parasitic blepharitis can also contribute to recurrent styes and inflammation.
Causes of Blepharitis (Eyelid Inflammation)
• Below we have mentioned some of blepharitis causes: • Infection e.g. Bacterial or parasitic infection. • Seborrheic tendency of individual (some individuals are prone for dandruff formation over scalp etc).
What Are the Risk Factors for Developing Blepharitis?
• Blepharitis can affect anyone, but certain factors increase the likelihood of developing the condition. Understanding these risk factors can help in early prevention and management.
1. Skin Conditions
Individuals with seborrheic dermatitis, rosacea, or eczema are at a higher risk of developing seborrheic blepharitis due to excessive oil production and inflammation around the eyelids.
2. Bacterial Infections
Staphylococcal blepharitis is often caused by bacterial overgrowth along the eyelid margins. People prone to staph infections or chronic eye irritation are more susceptible to this type of blepharitis.
3. Poor Eyelid Hygiene
Not cleaning the eyelids properly can lead to a buildup of debris, bacteria, and oil, which increases the risk of Meibomian blepharitis and ulcerative blepharitis.
4. Contact Lens Wearers
Frequent use of contact lenses, especially without proper hygiene, can contribute to posterior blepharitis due to increased bacterial accumulation and gland dysfunction.
5. Meibomian Gland Dysfunction (MGD)
Dysfunction of the Meibomian glands leads to blocked oil flow, which is a major contributor to posterior blepharitis and dry eye syndrome.
6. Mite Infestations (Demodex Blepharitis)
A high population of Demodex mites on the eyelashes can trigger demodex blepharitis, leading to inflammation, irritation, and crusting of the eyelids.
7. Hormonal Imbalances & Age
Aging leads to decreased oil production in the Meibomian glands, making Meibomian blepharitis more common in older adults. Hormonal changes can also contribute to gland dysfunction.
8. Environmental Factors
Exposure to dust, smoke, allergens, and pollution can aggravate the eyelids and increase the risk of allergic or irritant-induced blepharitis.
9. Use of Eye Makeup
Frequent use of eye makeup, mascara, and eyeliner without proper removal can clog the oil glands and trap bacteria, increasing the risk of anterior blepharitis.
10. Chronic Dry Eye Disease
Dry eye sufferers often experience posterior blepharitis as inadequate tear production leads to inflammation of the eyelid margins. Using the best eye drops for blepharitis can help manage this condition.
By identifying these risk factors, individuals can take proactive steps such as maintaining proper eyelid hygiene, using blepharitis medication when needed, and seeking medical advice for underlying conditions.
How to Relieve Itching Eyelids?
• Managing itchy eyelids involves proper blepharitis treatment, including:
• Eyelid hygiene: Regularly cleaning the eyelids with warm water and a gentle cleanser helps remove crust and bacteria.
• Blepharitis eye drops: Lubricating drops help soothe irritation and prevent dry eye symptoms.
• Blepharitis medication: Antibiotic or anti-inflammatory treatments may be prescribed for severe cases.
• Warm compresses: This helps open blocked oil glands, especially in posterior blepharitis.
By following these measures, itching eyelids caused by blepharitis can be effectively controlled, improving eye comfort and reducing inflammation.
- What is Diabetic Retinopathy?
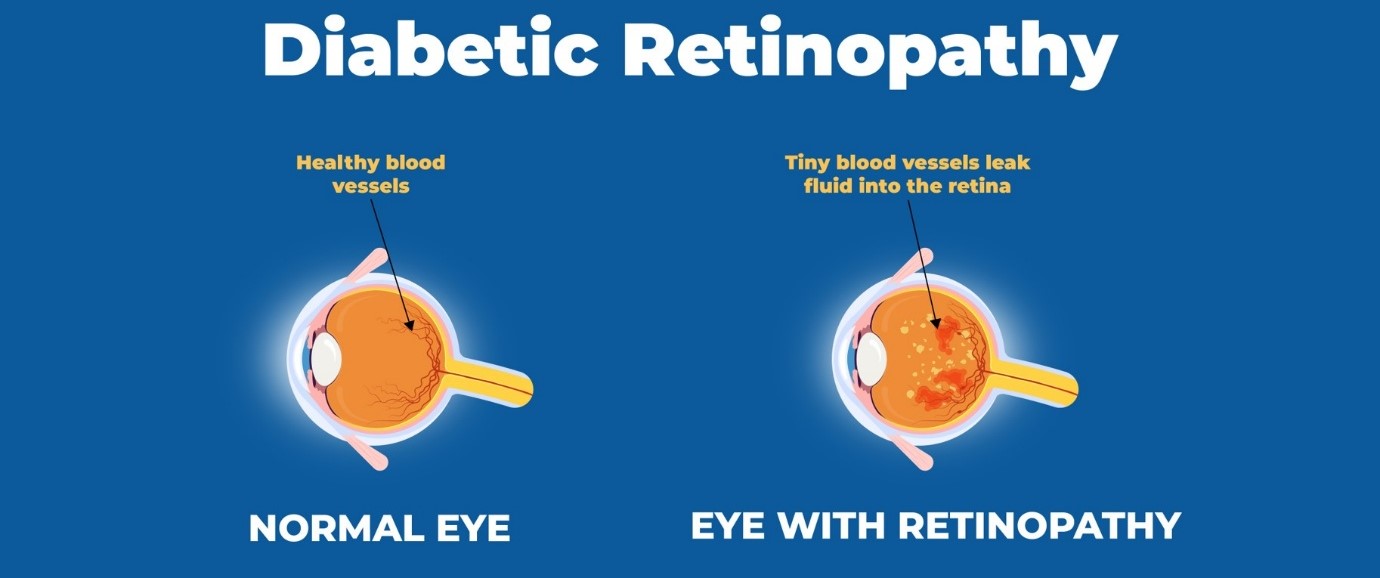
• Diabetic Retinopathy is a serious diabetes-related eye condition that affects the retina, the light-sensitive tissue at the back of the eye. It occurs when high blood sugar levels damage the small blood vessels in the retina, leading to vision impairment and, in severe cases, blindness. This condition progresses gradually, often without noticeable symptoms in the early stages, making regular eye checkups crucial for early detection and management.
Symptoms of Diabetic Retinopathy
The signs of diabetic retinopathy often don’t appear until significant damage has occurred inside the eye. Recognizing the symptoms early can help prevent severe vision loss.
1. Blurred Vision or Loss of Vision
As the diabetic retinopathy stages progress, the damaged blood vessels may leak fluid into the retina, causing blurred vision.
2. Seeing Floaters or Dark Spots
Dark spots or floaters appear when bleeding occurs inside the eye due to diabetic retinopathy, blocking light from reaching the retina.
3. Difficulty Seeing at Night
Patients may struggle with night vision due to decreased light sensitivity, which is one of the signs of diabetic retinopathy.
4. Difficulty Distinguishing Colors
As retinal cells become damaged, it may become challenging to differentiate between colors

Causes of Diabetic Retinopathy?
The primary diabetic retinopathy causes include prolonged high blood sugar levels and associated conditions.
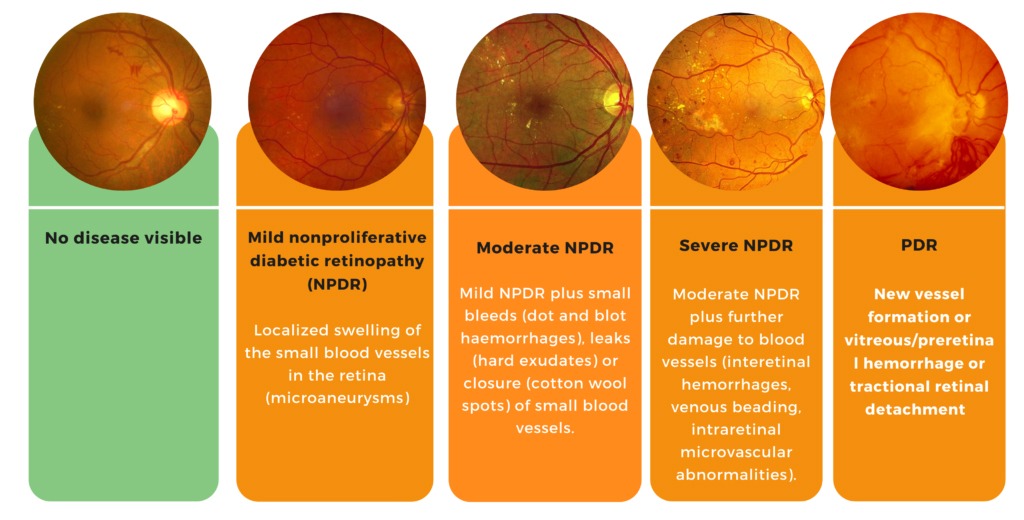
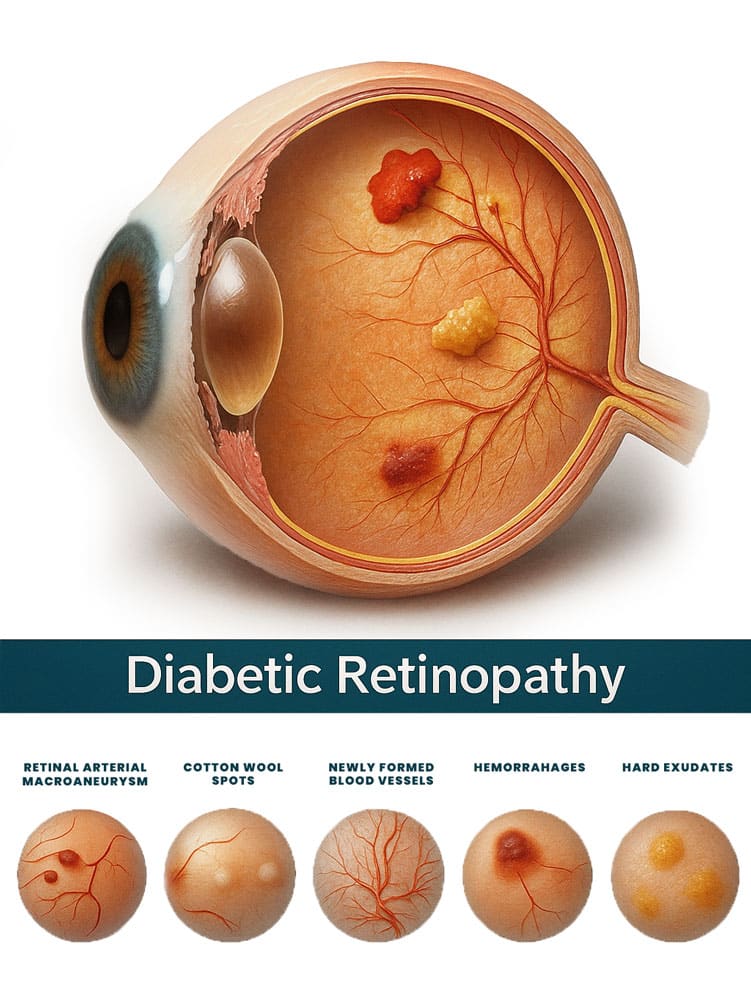
Stages of Diabetic Retinopathy
The damage occurs in four stages:
1. Mild Nonproliferative Retinopathy: Small bulges form in the blood vessels, causing leakage.
2. Moderate Nonproliferative Retinopathy: Blood vessels swell and distort, further restricting blood flow.
3. Severe Nonproliferative Retinopathy: Blocked blood vessels deprive the retina of oxygen, leading to new, fragile vessel growth.
4. Proliferative Diabetic Retinopathy:Advanced stage where new blood vessels form abnormally, leading to severe vision impairment.
- Diabetic Retinopathy Risk Factors
Several factors increase the risk of developing diabetic retinopathy:
• Uncontrolled blood sugar levels
• High blood pressure and cholesterol
• Long-term diabetes (Type 1 or Type 2)
• Smoking and poor lifestyle habits
• Pregnancy-related diabetes (Gestational Diabetes) How to Prevent Diabetic Retinopathy?
Preventing diabetic retinopathy involves maintaining overall eye health and managing diabetes effectively:
• Control blood sugar levels through a healthy diet and medication.
• Monitor blood pressure and cholesterol to reduce strain on blood vessels.
• Have regular eye exams to detect early changes in the retina.
• Quit smoking to improve circulation and eye health
Management of Diabetic Retinopathy
Effective management of diabetic retinopathy depends on the severity of the condition:
• Mild cases require regular monitoring and blood sugar control.
• Moderate to severe cases may require laser therapy or injections to reduce swelling.
• Advanced cases often require vitrectomy surgery to remove blood and prevent retinal detachment.- What is a Macular hole?
A macular hole is a small break or defect in the macula, the central part of the retina responsible for sharp, detailed vision. The macula is crucial for performing daily tasks such as reading, driving, recognizing faces, and distinguishing fine details. When a hole forms in this region, it disrupts central vision, causing blurring, distortion, and, in advanced cases, a significant reduction in sight.
The condition primarily affects older adults, typically over the age of 60, and is often associated with changes in the vitreous, the gel-like substance inside the eye. As people age, the vitreous shrinks and pulls away from the retina, sometimes creating tension on the macula and leading to the development of a hole.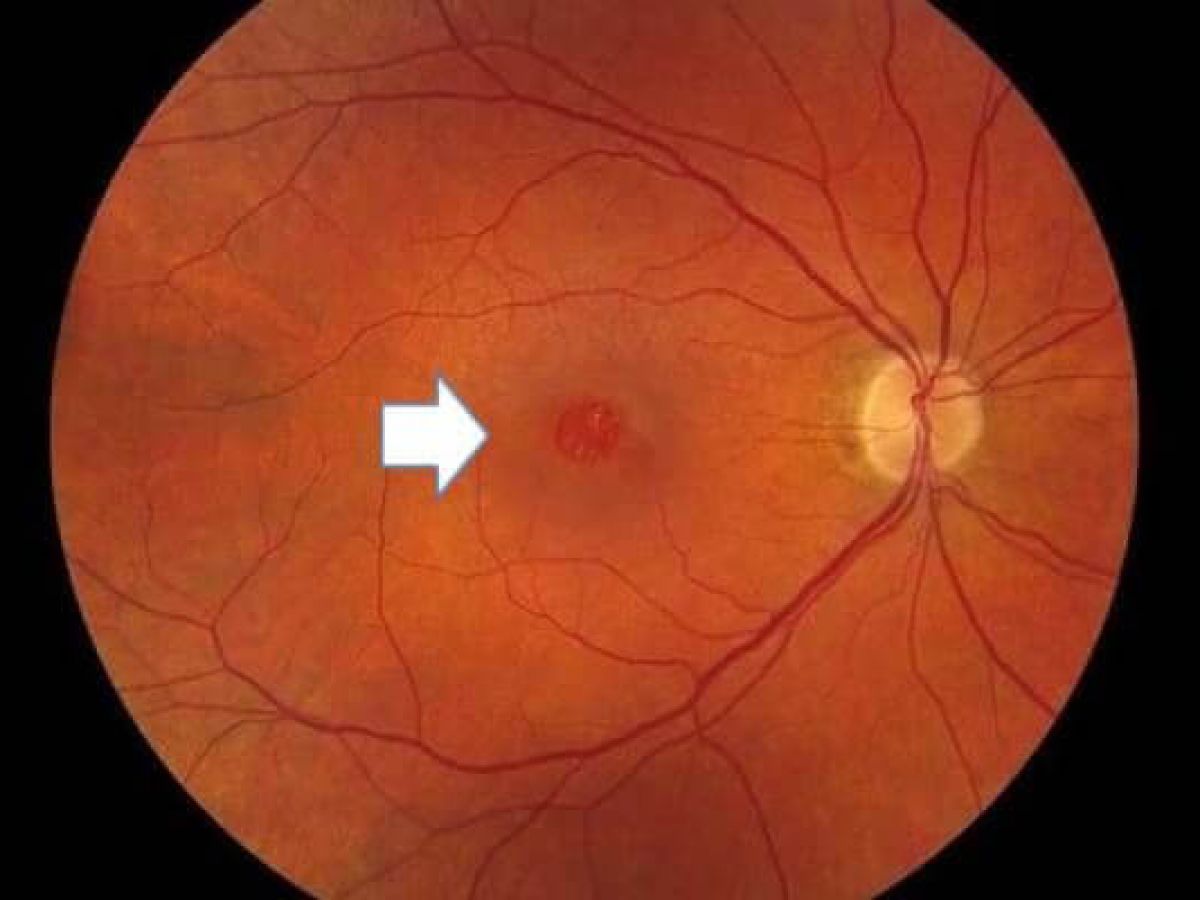
Macular Hole Symptoms
• Blurred or Distorted Vision –Straight lines may appear wavy or bent.
• Central Vision Loss –dark or blind spot in the center of vision.
• Difficulty Reading or Recognizing Faces –Fine details become hard to see.
• Increased Light Sensitivity –Bright lights may cause discomfort.
• Reduced Sharpness and Clarity –Vision appears hazy or unclear.
• Objects Appear Smaller or Further Away –A phenomenon called micropsia.

Causes of Macular Hole
• A macular hole is a small break or defect in the macula, the central part of the retina responsible for sharp, detailed vision. It can cause blurry or distorted central vision. Several factors can contribute to its development:
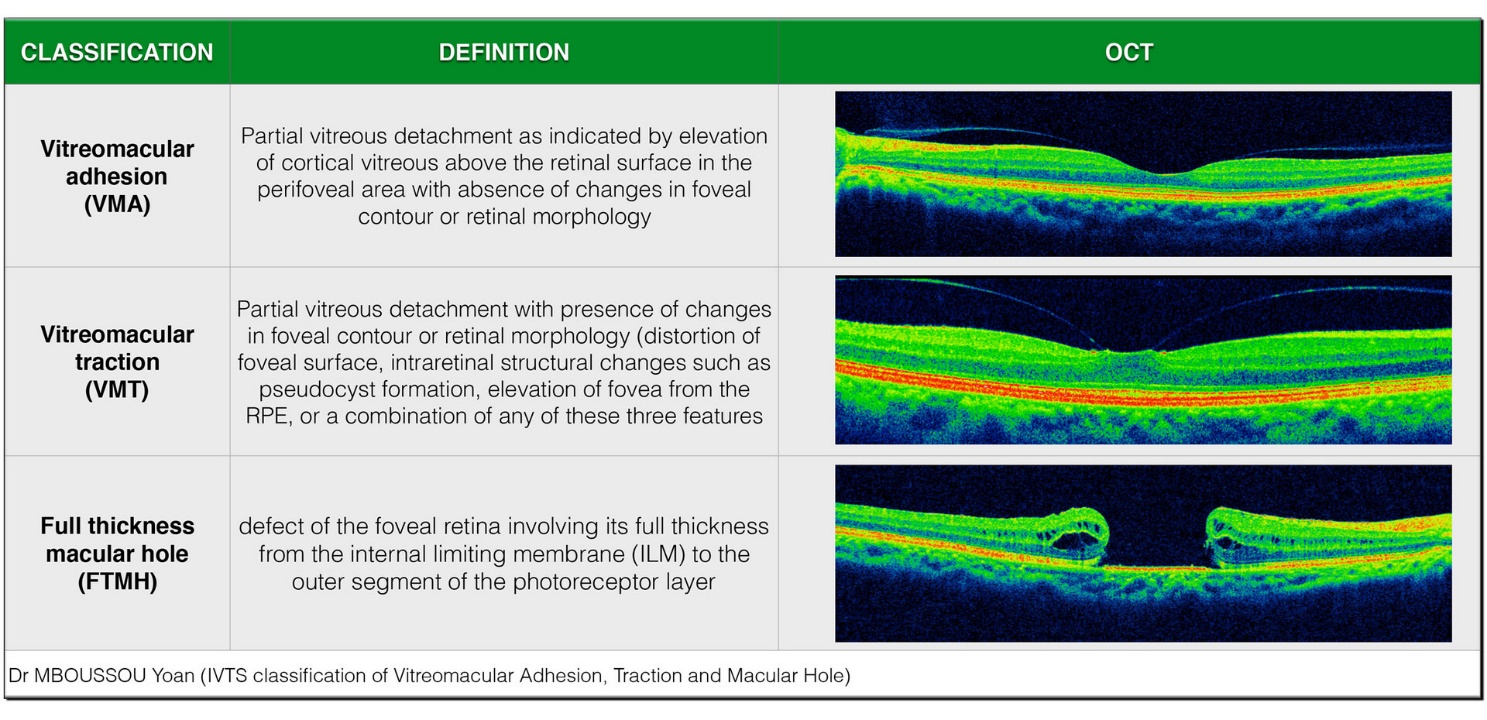
Primary Causes:
1. Aging (Vitreo-Macular Traction) – The most common cause. As we age, the vitreous gel inside the eye shrinks and pulls away from the retina. If it adheres to the macula too strongly, it can create a hole.
2. High Myopia (Severe Nearsightedness) – People with high myopia have thinner retinas, making them more susceptible to macular holes.
3. Trauma or Injury – Direct trauma to the eye, such as a blow or accident, can cause a macular hole.
4. Retinal Detachment or Epiretinal Membrane – Conditions that cause traction or pulling on the retina may lead to a macular hole.
5. Diabetic Eye Disease – Severe diabetic retinopathy can weaken the macula, increasing the risk of holes forming.
6. Macular Edema (Swelling of the Macula) – Fluid buildup can weaken the macular tissue, leading to hole formation.
Less Common Causes:
1. Inflammatory Diseases (such as uveitis)
2. Macular Telangiectasia (a rare retinal disorder)
3. Previous Eye Surgery (like cataract or retinal surgery, which can sometimes lead to macular holes
Who is at Risk of Developing a Macular Hole?
Certain factors can increase the likelihood of developing a macular hole, including:
• Aging: The primary risk factor, as macular holes predominantly affect individuals over 60.
• Gender: Women are at a slightly higher risk than men, though the reason is not entirely understood.
• High Myopia (Severe Nearsightedness): People with extreme myopia experience thinning of the retina, increasing the risk of developing a macular hole.
• Eye Trauma: Injuries from blunt force, sports, accidents, or any direct impact to the eye can lead to retinal damage and macular hole formation.
• Diabetic Retinopathy: Long-standing diabetes can lead to structural retinal changes that may predispose individuals to macular holes.
• Previous Retinal Detachment Surgery: Individuals who have undergone procedures to treat retinal detachment may be at higher risk.
• Vitreous Shrinkage or Detachment: As the eye ages, the vitreous contracts and pulls away from the retina. If the adhesion is too strong, it can create a hole.
• Genetics and Family History: Though less common, a hereditary component may exist, increasing susceptibility to macular holes.- Stye Explained: Causes, Symptoms, Treatments, and Prevention
A stye is a painful, swollen bump that appears on the edge of the eyelid due to a bacterial infection of the oil glands. Known medically as hordeolum, this common condition can cause discomfort, redness, and irritation. Styes can occur in various locations, such as inside the eyelid, under the eye, or along the eyelash line.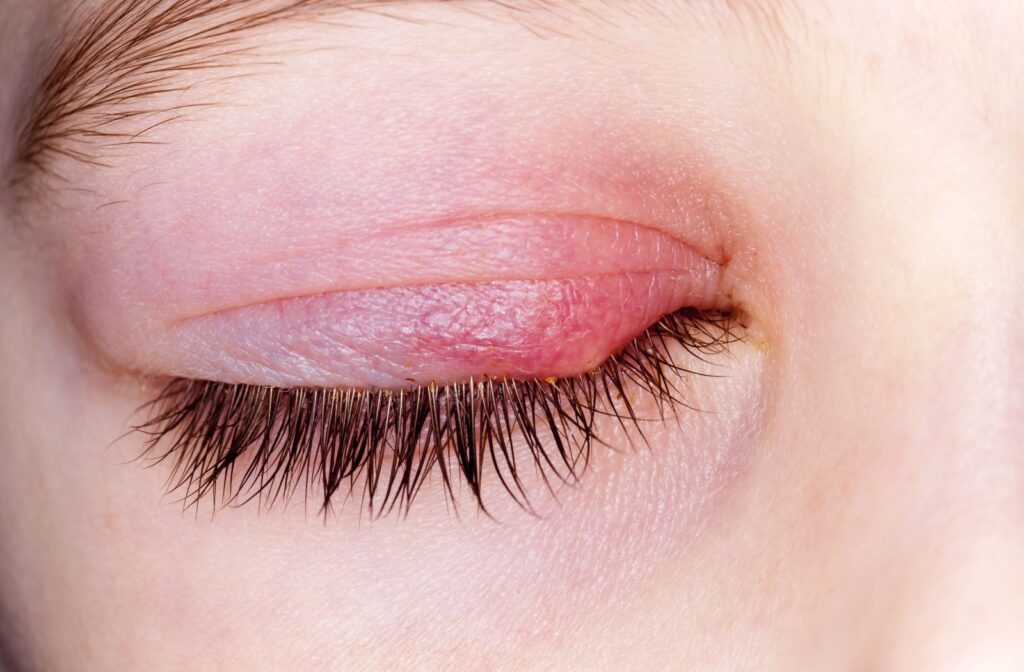
What is a Stye?
A stye is a localized bacterial infection that forms near the base of an eyelash or inside an oil gland in the eyelid. These infections occur when bacteria, usually Staphylococcus aureus, enter the glands and cause inflammation. Styes can be classified into different types based on their location: • External Stye (Hordeolum Externum): Forms along the outer edge of the eyelid, often due to an infection of an eyelash follicle.
• Internal Stye (Hordeolum Internum): Develops inside the eyelid when the meibomian glands become infected.
• Stye inside the eyelid: This type of stye is less visible but can cause significant discomfort.
• Eye stye under eyelid: These can create a sensation of something stuck in the eye.
• Stye under the eye: Affects the lower eyelid and may cause redness and tenderness. Causes of Styes
The causes of a stye revolve around bacterial infections and blockages in the oil glands. Several risk factors can contribute to their development:
1. Bacterial Infection
Styes are most commonly caused by Staphylococcus bacteria, which naturally reside on the skin. When these bacteria infect an oil gland or hair follicle, a stye forms.
2. Poor Eyelid Hygiene
Failing to wash your hands before touching your face, using expired makeup, or neglecting to clean contact lenses can introduce bacteria to the eyes, increasing the risk of infection.
3. Blocked Oil Glands
The tiny oil glands along the eyelid, known as meibomian glands, can become clogged due to excess oil, dirt, or debris. A blockage can create a breeding ground for bacteria, leading to a stye.
4. Frequent Eye Rubbing
Rubbing your eyes with unclean hands can transfer bacteria to the eyelids, increasing the likelihood of infection.
5. Chronic Blepharitis
Blepharitis is a condition that causes inflammation of the eyelids. Those with chronic blepharitis are more likely to develop recurrent styes.
6. Weakened Immune System
A weakened immune system due to stress, lack of sleep, or illness can make a person more susceptible to bacterial infections, including styes.
Symptoms of a Stye
The symptoms of a stye can vary depending on the severity of the infection, but common signs include:
• A red, swollen bump on the eyelid
• Pain and tenderness around the affected area
• A burning or itching sensation in the eye
• Excessive tearing
• Light sensitivity
• Crusting around the eyelid margin
• A pus-filled centre, which may eventually rupture and drain
How to Treat a Stye
Most styes resolve on their own within a week, but several treatment options can help speed up recovery and reduce discomfort.
1. Warm Compress
Applying a warm compress for 10-15 minutes, three to four times a day helps soften the stye, reduce swelling, and encourage drainage.
2. Maintain Eyelid Hygiene
• Wash hands before touching your eyes.
• Use a mild baby shampoo or eyelid cleanser to clean the affected area.
3. Avoid Squeezing the Stye
Never pop or squeeze a stye, as this can spread the infection and worsen the condition.
4. Over-the-Counter Treatments
• Antibiotic eye drops and ointment can help reduce bacterial growth.
• Pain relievers like ibuprofen can alleviate discomfort.
5. Medical Intervention
If a stye persists beyond 5 days or becomes extremely painful, an eye doctor may drain it or prescribe antibiotics.
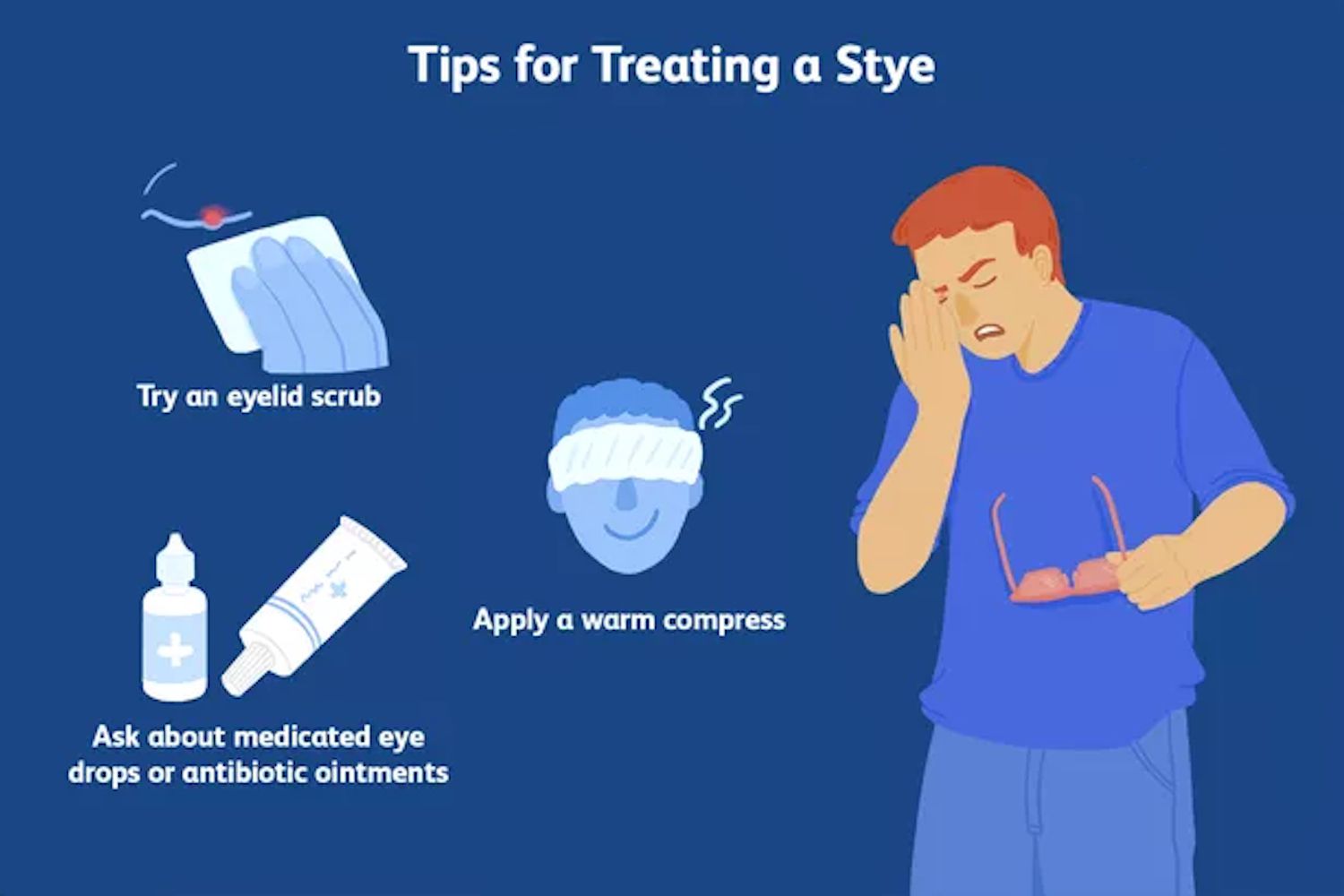
Preventing Styes
To reduce the risk of developing a stye, follow these preventive measures:
• Wash your hands frequently to avoid transferring bacteria to your eyes.
• Avoid sharing makeup or personal eye care products.
• Replace old eye makeup every three to six months.
• Clean your contact lenses properly and avoid sleeping with them.
• Manage blepharitis if you have chronic eyelid inflammation.
• Eat a healthy diet and get enough sleep to strengthen your immune system.- Understanding Myopia: What Causes It?

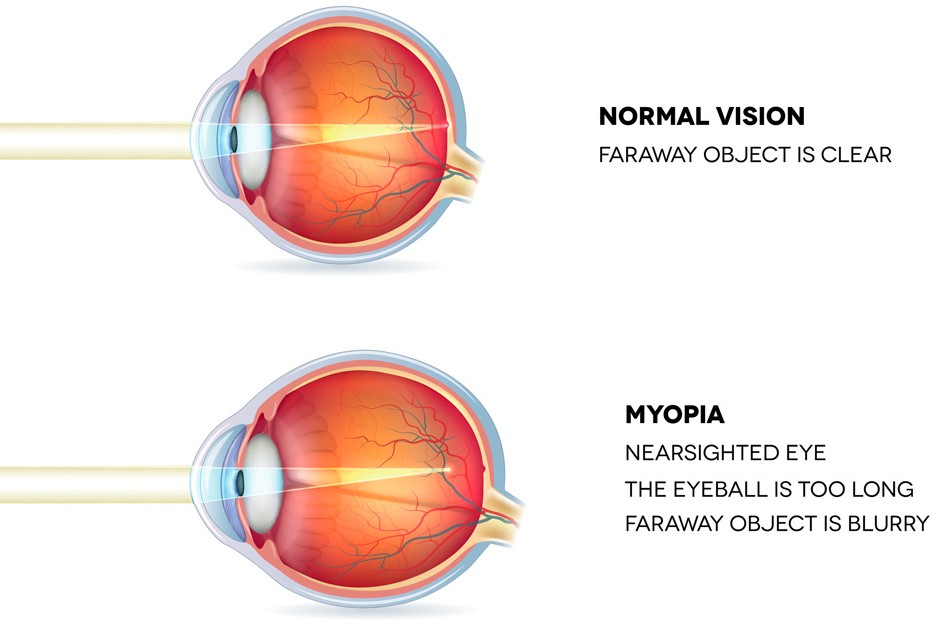 Myopia is primarily caused by the elongation of the eyeball, which alters how light enters and focuses on the retina. Several factors contribute to its development, including:
Myopia is primarily caused by the elongation of the eyeball, which alters how light enters and focuses on the retina. Several factors contribute to its development, including:
• Genetics:
If one or both parents have myopia, there is a higher likelihood of developing it.
• Prolonged Near Work:
Excessive screen time, reading, or close-up work can increase the risk of myopia progression.
• Lack of Outdoor Activities:
Studies suggest that children who spend less time outdoors are more prone to developing myopia.
• Poor Lighting Conditions:
Insufficient lighting while reading or working on screens can strain the eyes and contribute to myopia
Symptoms and signs of myopia


Treatment Options for Myopia (Nearsightedness)
There are several treatment options for myopia (nearsightedness) that help improve vision clarity and reduce dependency on corrective lenses. These options include non-surgical treatments such as corrective lenses and specialized eye exercises, as well as surgical interventions for those seeking a more permanent solution. Non-Surgical Treatment Options for Myopia
1. Prescription Eyeglasses Eyeglasses are the most common and non-invasive solution for myopia. They correct refractive errors by adjusting how light focuses on the retina. There are different types of lenses used for myopia correction, including:
• Single Vision Lenses – Corrects distance vision.
• Bifocal or Progressive Lenses – Suitable for individuals who need both near and distance vision correction.

2. Contact Lenses
For those who prefer an alternative to glasses, contact lenses provide effective myopia correction by sitting directly on the eye’s surface. Types of contact lenses for myopia include:
• Soft Contact Lenses – Comfortable and widely used.
• Rigid Gas Permeable (RGP) Lenses – Provide sharper vision and are ideal for high myopia.
• Orthokeratology (Ortho-K) Lenses – Special overnight lenses that reshape the cornea temporarily to provide clear daytime vision.
• Palming technique to relax eye muscles.

3. Atropine Eye Drops
Low-dose atropine eye drops have been shown to slow the progression of progressive myopia in children. These drops help reduce eye elongation, a major cause of worsening myopia.
4. Myopia Control Glasses or Contact Lenses
Specialized myopia control lenses help slow down myopia progression, especially in children.
5. Eye Exercises for Myopia
Although eye exercises cannot reverse myopia, they help in reducing eye strain and improving focus flexibility. Some common exercises include:
• Blinking exercises to prevent dry eyes from excessive screen time.
• Focus shifting between near and distant objects.
• Palming technique to relax eye muscles.

Surgical Options for Myopia Correction
For those looking for long-term solutions, surgical interventions are available to correct myopia permanently. These procedures reshape the cornea to improve how light focuses on the retina.
1. LASIK (Laser-Assisted in Situ Keratomileusis)
LASIK is the most popular laser eye surgery for myopia correction. It involves reshaping the cornea to allow light to focus directly on the retina, leading to clearer vision.
• Pros: Quick recovery, minimal discomfort, effective for moderate myopia.
• Cons: Not suitable for individuals with very thin corneas or severe myopia.
2. PRK (Photorefractive Keratectomy)
PRK is an alternative to LASIK for those with thin corneas. Instead of creating a corneal flap, the outermost layer of the cornea is removed, and laser treatment is applied to reshape the cornea.
• Pros: Effective for those unsuitable for LASIK.
• Cons: Longer recovery time compared to LASIK.

3. SMILE (Small Incision Lenticule Extraction)
SMILE surgery is a minimally invasive laser procedure where a small disc of corneal tissue is removed through a keyhole incision to correct myopia.
• Pros: Faster recovery and less dry eye than LASIK.
• Cons: Limited suitability for very high myopia.
4. Implantable Collamer Lenses (ICL)
ICL surgery involves implanting a corrective lens inside the eye to treat high myopia. Unlike LASIK, no corneal tissue is removed.
• Pros: Reversible and suitable for extreme myopia.
• Cons: Involves a slightly higher risk than LASIK.
5. Refractive Lens Exchange (RLE)
This procedure is similar to cataract surgery, where the natural eye lens is replaced with an artificial intraocular lens (IOL) to correct myopia.
• Pros: Ideal for older individuals with high myopia.
• Cons: Not recommended for younger patients.
- What is Glaucoma
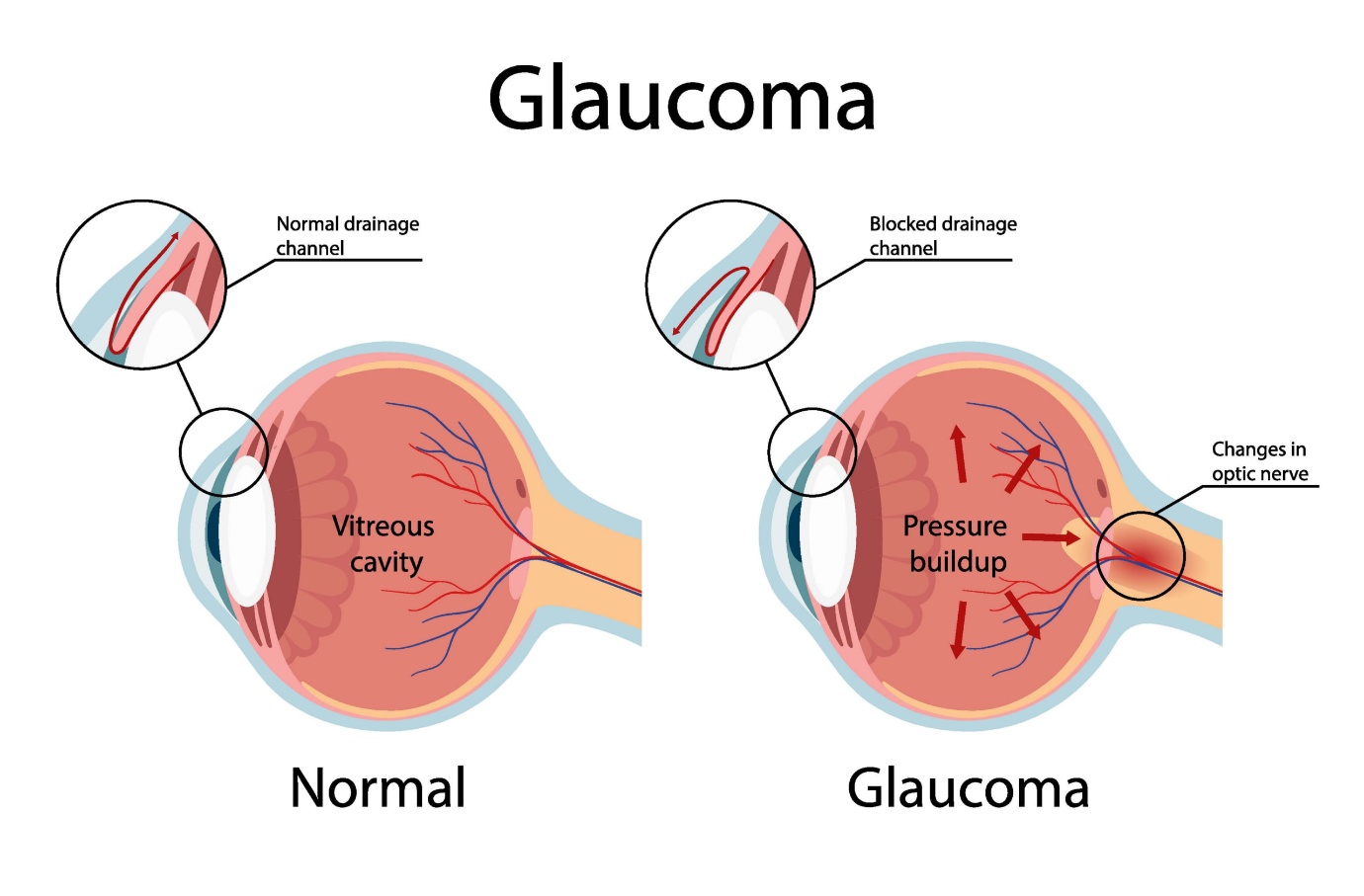
Glaucoma is a silent thief of sight—one of the leading causes of irreversible blindness worldwide. This progressive eye disease damages the optic nerve due to increased intraocular pressure, leading to gradual vision loss. The most alarming part? It often creeps in without noticeable symptoms until significant damage is done. Understanding glaucoma, its causes, symptoms, and prevention methods can help safeguard your vision.

What Are the Symptoms of Glaucoma?
Glaucoma symptoms vary depending on the type and severity of the condition. While some people may experience gradual vision changes, others may notice sudden and severe symptoms. Below are the warning signs:
1. Loss of Vision
One of the most significant indicators of glaucoma is glaucoma vision deterioration, where blind spots appear in peripheral or central vision.
2. Blurry Vision
Blurred or hazy vision is an early warning sign, especially in angle-closure glaucoma where the pressure spikes suddenly.
3. Persistent Headache
High intraocular pressure can lead to intense headaches, often accompanied by eye pain.
4. Eye Redness
Redness in the eye is another symptom of glaucoma disease, indicating increased intraocular pressure or inflammation.
5. Stomach Upset, Nausea, and Vomiting
In acute cases, sudden pressure spikes can lead to nausea and vomiting, often misattributed to other conditions.
6. Pain in the Eye
Discomfort or severe pain in the eye may indicate phacolytic glaucoma or phacomorphic glaucoma, where lens changes obstruct normal fluid drainage.
7. Early Presbyopia
Difficulty focusing on nearby objects may suggest early onset of eye disorders linked to glaucoma.

Causes of Glaucoma
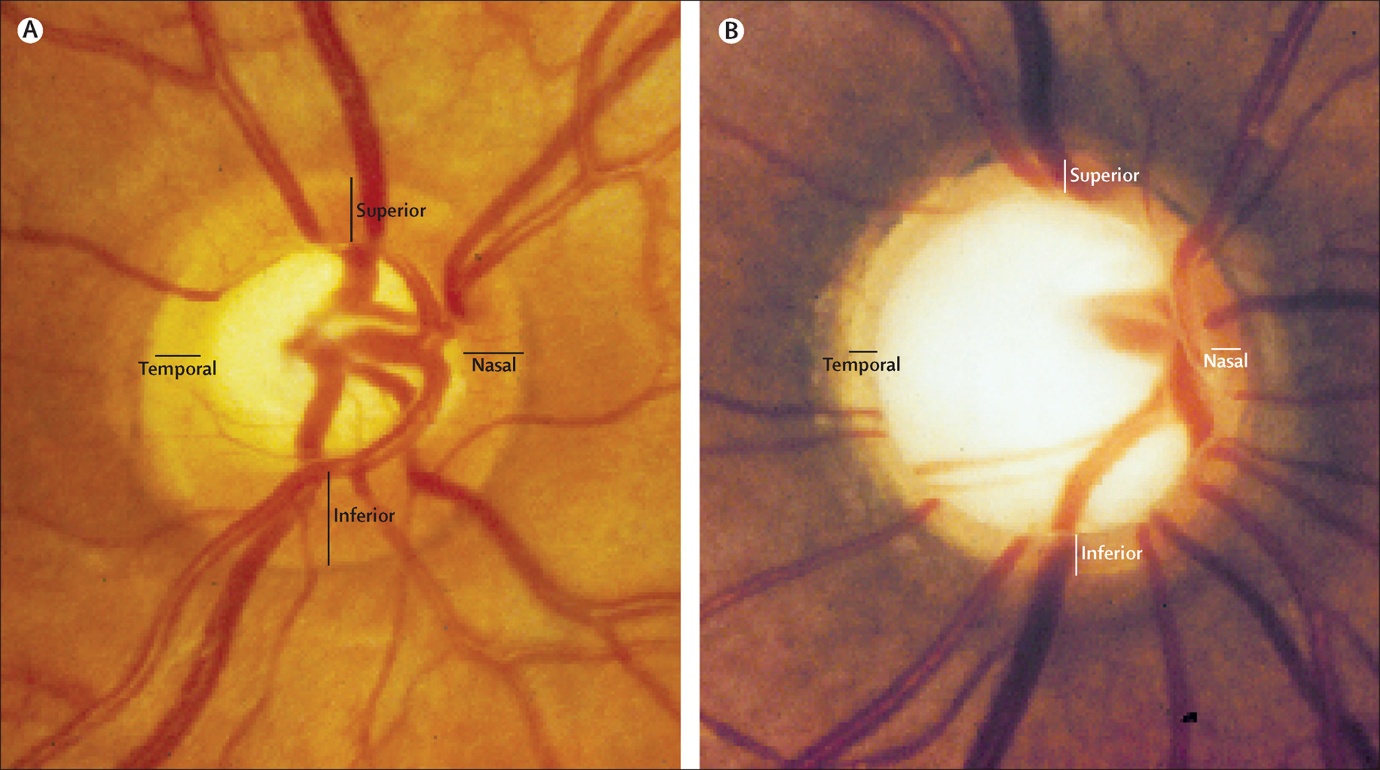
1. Build-up of Aqueous Humor Inside the Eye
The eye maintains internal pressure by producing and draining aqueous humor. A blockage in this drainage system can lead to excessive pressure.
2. Genetic Reasons
Family history significantly increases the risk of developing glaucoma symptoms over time.
3. Birth Defects
Congenital defects in the eye’s drainage system can cause childhood glaucoma.
4. Blunt or Chemical Injury
Trauma or exposure to harmful chemicals can disrupt the normal flow of fluids inside the eye.
5. Acute Eye Infection
Certain infections cause inflammation and scarring, leading to glaucoma disease.
6. Blockage by Blood Vessels Inside the Eye
Poor circulation can cause vessel blockages, increasing the risk of glaucoma vision loss.
7. Inflammatory Conditions
Autoimmune diseases like uveitis can trigger secondary glaucoma.
Glaucoma Risk Factors
Are you at risk? Identifying these factors can help with early detection and prevention.
1. Are You Over 60 Years of Age?
Age is a significant risk factor, as the drainage system naturally weakens over time.
2. Have High Internal Eye Pressure?
Elevated intraocular pressure is a primary contributor to glaucoma.
3. Have a Family Member Diagnosed with Glaucoma?
A strong genetic link exists, making family history a key risk factor.
4. Have Certain Medical Conditions?
Diabetes, hypertension, and anaemia increase glaucoma susceptibility.
5. Have Thin Corneas?
Thin corneas lead to inaccurate pressure readings, masking high intraocular pressure.
6. Have Extreme Near-sightedness or Farsightedness?
Severe refractive errors alter the eye’s anatomy, increasing glaucoma risk.
7. Have Had Eye Injuries or Surgeries?
Trauma and surgical procedures can alter fluid dynamics inside the eye.
8. Taking Corticosteroids for a Long Time?
Prolonged steroid use can trigger secondary glaucoma.

How to Prevent Glaucoma
While glaucoma cannot be completely prevented, early detection and lifestyle changes can slow its progression.
1. Have Eye Checkups Often
Routine exams help detect glaucoma symptoms before irreversible damage occurs.
2. Be Aware of Your Family’s Medical History
If glaucoma runs in your family, regular screenings are essential.
3. Keep Fit and Eat Healthy
A diet rich in leafy greens, omega-3 fatty acids, and antioxidants promotes eye health.
4. Protect Your Eyes While Performing Tasks That Could Cause Injuries
Wearing protective eyewear during sports or hazardous activities prevents trauma-induced glaucoma.
Glaucoma is a serious but manageable condition if diagnosed early. Prioritizing regular eye exams, understanding risk factors, and taking preventive measures can help protect your sight. If you experience any glaucoma symptoms, consult an eye specialist immediately.
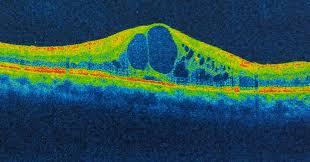
- What is Macular Edema?
 The macula, a critical part of the retina, is essential for sharp central vision, enabling us to see fine details, recognise distant objects, and perceive colours with accuracy. This makes it central to understanding macular oedema.
Macular edema occurs when abnormal fluid builds up in the macula, causing it to swell. This often leads to blurred central vision and difficulties with daily activities such as reading, driving, or recognising faces.
Symptoms of Macular Edema
The macula, a critical part of the retina, is essential for sharp central vision, enabling us to see fine details, recognise distant objects, and perceive colours with accuracy. This makes it central to understanding macular oedema.
Macular edema occurs when abnormal fluid builds up in the macula, causing it to swell. This often leads to blurred central vision and difficulties with daily activities such as reading, driving, or recognising faces.
Symptoms of Macular Edema

Macular edema is usually painless and often goes unnoticed in the early stages, making it challenging for patients to recognise until vision problems become more apparent.
• Blurred or wavy central vision
Intravitreal injections of Anti-VEGF medicines work by inhibiting the growth of abnormal blood vessels in the retina, reducing leakage and stabilising vision. These treatments have shown significant success in improving visual outcomes for patients with macular edema.
• Colors may appear different
• May experience difficulty in reading
Symptoms of Macular Edema

Macular edema is usually painless and often goes unnoticed in the early stages, making it challenging for patients to recognise until vision problems become more apparent.
• Blurred or wavy central vision
Intravitreal injections of Anti-VEGF medicines work by inhibiting the growth of abnormal blood vessels in the retina, reducing leakage and stabilising vision. These treatments have shown significant success in improving visual outcomes for patients with macular edema.
• Colors may appear different
• May experience difficulty in reading
Causes of Macular Edema
Macular edema can occur due to several underlying eye and systemic conditions. In diabetes, prolonged high blood sugar levels can weaken and damage retinal blood vessels, leading to fluid leakage into the macula and subsequent swelling.
• Diabetes:
Hypertension (high blood pressure) can also contribute by leading to retinal vein occlusions, which block normal blood flow and trigger fluid accumulation. Additionally, age-related macular degeneration (AMD) is another common cause, where degenerative changes in the macula damage blood vessels, allowing fluid or blood to leak and impair central vision.
A routine dilated fundus examination conducted by an experienced ophthalmologist is vital for diagnosing macular edema, as it provides a clear view of the retina and helps detect early fluid leakage or swelling.
Certain drugs, including some used for cancer treatment or eye therapies, can occasionally lead to macular edema as a side effect. Patients should always share their medication history with their ophthalmologist to assess and minimise risks.
• Age related Macular Degeneration:
Here abnormal blood vessels leak fluid and cause macular swelling.
• Retinal Vein oclussions:
When the veins in the retina become blocked,blood and fluid then leak out into the macula.
• Vitreomacular traction(VMT)
• Genetic/Hereditary disorders:
such as Retinoschisis or Retinitis Pigmentosa.
• Inflammatory eye diseases:
Conditions like uveitis, where the body attacks its own tissues, can damage retinal blood vessels and cause swelling of the macula.
• Medication:
Certain drugs, such as those used for treating cancer or eye conditions, can cause side effects like macular edema in rare cases. It’s important for patients to discuss their medication history with their doctor to minimize risks.
• Eye Malignancies:
Both benign and malignant tumors can lead to macular edema.
• Eye surgery:
It’s not common, but sometimes after glaucome, retinal or cataract surgery, you can get macular edema.
• Injuries:
Trauma to the eye.
Macular Edema Risk Factors
• Metabolic conditions (diabetes)
• Blood vessel diseases (vein occlusion/blockage)
• Aging (macular degeneration)
• Hereditary diseases (retinitis pigmentosa)
• Traction on the macula (macular hole, macular pucker, and vitreomacular traction)
• Inflammatory conditions (sarcoidosis, uveitis)
• Toxicity
• Neoplastic conditions (eye tumors)
• Trauma
• Surgical causes (following eye surgery)
• Unknown (idiopathic) causes
Macular Edema Prevention
Anyone with diabetes should have their eyes checked annually, at the least. People with family history or underlying genetic condition can have a yearly eye examination.
- What is Squint (Strabismus)?

Squint, also known as strabismus, is a condition where the eyes do not align properly. One eye may turn inward, outward, upward, or downward while the other eye remains focused. This misalignment can be constant or occasional, affecting depth perception and overall vision. Squint can occur in children and adults, leading to vision disturbances, eye strain, and even permanent vision loss if left untreated.
Symptoms of Squint (Strabismus)
The symptoms of squint vary depending on the severity and type of misalignment. Some common signs include:
• Misaligned eyes (one eye turning in a different direction)
• Double vision
• Difficulty focusing on objects
• Frequent eye strain or headaches
• Squinting or tilting the head to see clearly
• Reduced depth perception
• Inconsistent vision clarity
Causes of Squint (Strabismus)
Squint can develop due to various reasons, including:
• Genetic factors : A family history of squint increases the risk.
• Nerve disorders : Conditions affecting eye muscle control can lead to misalignment.
• Refractive errors : Uncorrected myopia, hyperopia, or astigmatism can cause the eyes to work harder, leading to squint.
• Eye muscle imbalances : Weakness or dysfunction in eye muscles can result in misalignment.
• Neurological conditions : Certain brain disorders may interfere with eye coordination.
• Injuries : Trauma affecting the eye muscles or nerves can cause squint.
• Medical conditions : Issues like cerebral palsy or Down syndrome are often associated with squint.

Squint Prevention
While some types of squint cannot be prevented, early detection and intervention can help reduce complications. Here are some preventive measures:
• Regular eye check-ups, especially in children
• Correcting refractive errors with glasses or contact lenses
• Managing underlying health conditions that may contribute to squint
• Eye exercises to strengthen coordination and alignment
• Encouraging proper screen time habits to reduce eye strain
- What is Retinal Detachment?
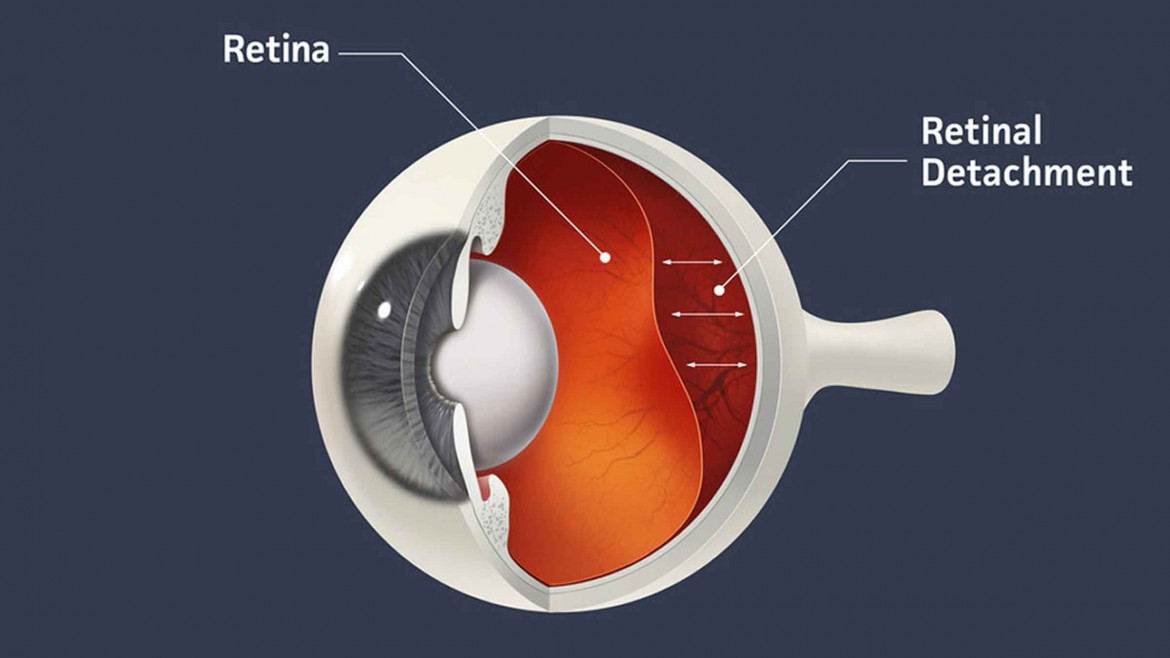
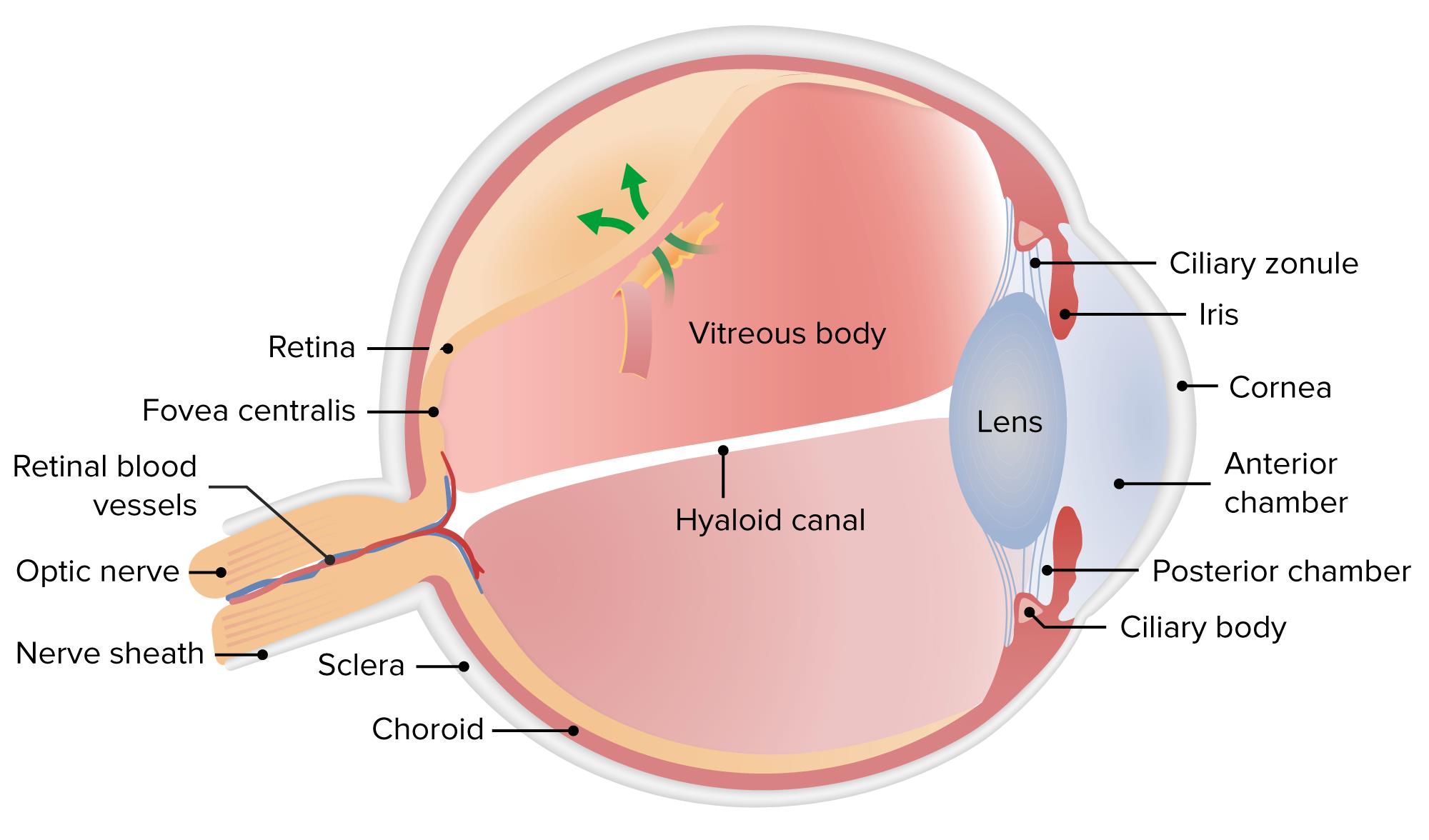
Retinal detachment is a serious eye condition in which the retina, the light-sensitive layer at the back of the eye, pulls away from its normal position. This separation prevents the retina from functioning properly, leading to vision impairment or blindness if left untreated. Common causes include aging, trauma, or underlying conditions like severe myopia. Early detection and prompt treatment are crucial to preventing permanent vision loss.
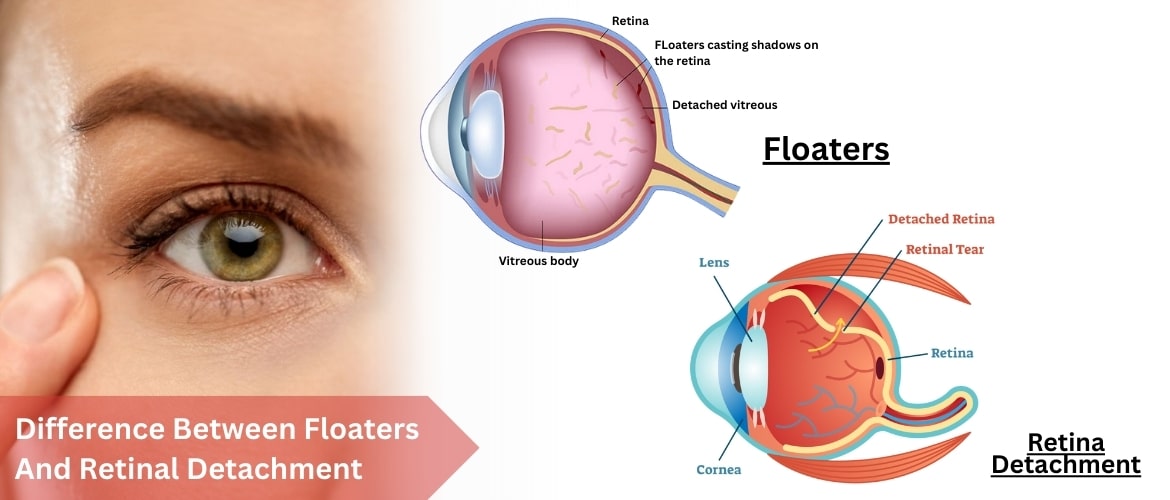


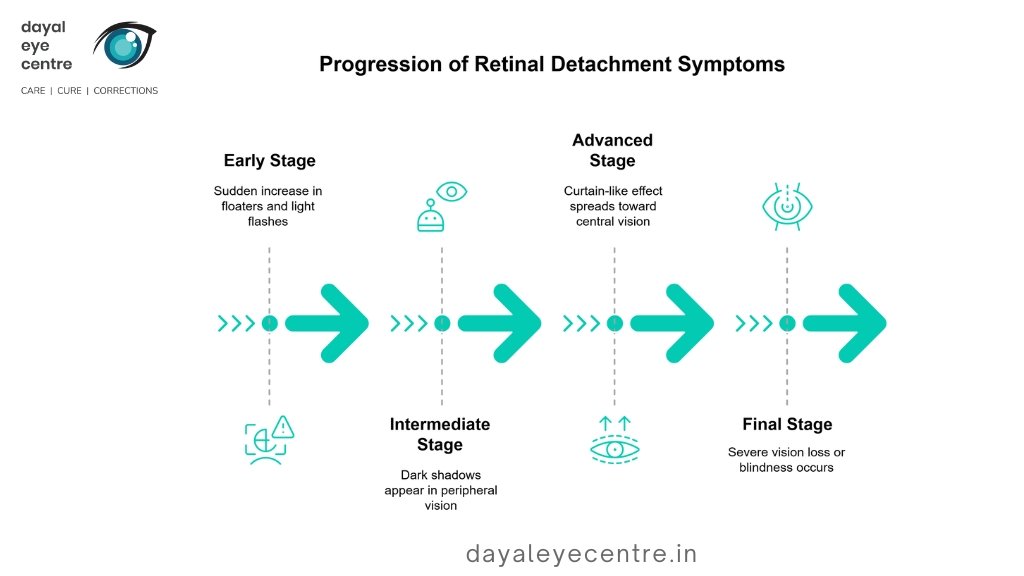
Retinal Detachment Symptoms
Recognizing the early warning signs of retinal detachment is crucial for timely medical intervention. Below are some of the key indicators:
• Flashes of Light (Photopsia)
One of the most common symptoms of retinal detachment is experiencing brief flashes of light, known as photopsia. These flashes typically occur in the extreme peripheral vision and are unrelated to external light sources. They may appear as sudden, bright flickers, resembling lightning streaks. While occasional flashes can be harmless, persistent or increasing occurrences may signal a retinal tear or detachment.
• Sudden Increase in Floaters Floaters are small, shadowy specks or thread-like shapes that move across your field of vision. While floaters are common with aging, a sudden and dramatic increase in their number could indicate retinal detachment. This happens when the vitreous gel inside the eye pulls away from the retina, sometimes leading to tears or breaks. Seeking immediate medical attention is recommended if new floaters appear alongside flashes of light.
• Ring of Floaters Near Central Vision
In some cases, people experience a concentration of floaters forming a ring-like pattern near the temporal side of their central vision. This symptom may be an early warning sign of a retinal tear before full detachment occurs. If left untreated, it can progress to severe vision impairment.
• Curtain or Shadow Over Vision
A significant symptom of retinal detachment is the appearance of a dark shadow or curtain descending over part of the visual field. This shadow may begin at the sides (peripheral vision) and gradually move toward the center, obstructing sight. It may also feel as though a veil is covering parts of the vision. This symptom usually indicates a progressing retinal detachment, requiring immediate medical intervention.
• Veil-Like Effect in the Field of Vision
Another striking symptom is the impression of a veil or curtain being drawn over the field of vision. This may occur suddenly or progress gradually, worsening over time. The severity depends on how much of the retina is affected. If ignored, this can lead to irreversible blindness.
• Distorted Vision (Metamorphopsia)
Retinal detachment can cause straight lines to appear bent, wavy, or distorted. This distortion occurs due to the retinal layers shifting from their normal position, affecting how light is processed. People may struggle to read, recognize faces, or see fine details. If macular involvement occurs, distortion may be severe and permanent if left untreated.
• Loss of Central Vision
As retinal detachment progresses, central vision may become blurry or disappear entirely. This happens when detachment spreads toward the macula, the part of the retina responsible for sharp, detailed vision. The extent of vision loss depends on the severity and duration of detachment. If the macula becomes fully detached, surgery must be performed urgently to restore vision, though full recovery may not always be possible.
Causes of Retinal Detachment
Retinal detachment can occur due to various underlying conditions and risk factors. The most common retinal detachment causes include severe myopia (nearsightedness), ocular trauma, previous eye surgeries, and diabetic retinopathy. Below are some of the major causes:
• Myopia (Nearsightedness) and Retinal Detachment
Severe myopia is a significant risk factor for retinal detachment. In individuals with high myopia, the eyeball is elongated, stretching the retina and making it thinner and more fragile. This increases the likelihood of retinal tears and lattice retinal degeneration, which can lead to retinal separation. Regular eye checkups are crucial for people with high myopia to monitor retinal health.
• Previous Cataract Surgery and Retinal Detachment
People who have undergone cataract surgery may have an increased risk of retinal detachment. During surgery, the natural lens is removed and replaced with an artificial intraocular lens (IOL). In some cases, this process can cause vitreous detachment, leading to retinal tears or exudative retinal detachment due to fluid accumulation. Patients who experience sudden retinal detachment eye flashes or floaters after cataract surgery should seek immediate medical attention.
• Ocular Trauma and Retinal Separation
Ocular trauma, including sports injuries, blunt force impacts, or accidents, can result in retinal detachment. A direct blow to the eye can cause the retina to tear or detach completely. Athletes and individuals in high-risk professions should use protective eyewear to minimize the chances of traumatic retinal detachment.
• Lattice Retinal Degeneration and Retinal Detachment
Lattice retinal degeneration is a condition where the peripheral retina becomes thinner and more vulnerable to tears. This degeneration is common in individuals with high myopia and can lead to spontaneous retinal detachment. Regular eye exams, including retinal detachment vision simulator tests, can help detect early signs of lattice degeneration and prevent serious complications.
• A Family History of Retinal Detachment
Genetics play a role in retinal detachment causes, as individuals with a family history of the condition are at higher risk. Certain inherited conditions, such as Stickler syndrome or Marfan syndrome, weaken retinal structures, increasing the chances of retinal separation. If there is a history of retinal detachment in the family, routine screenings are recommended to monitor retinal health.
• Diabetic Retinopathy and Retinal Detachment
Diabetes-related eye conditions, such as diabetic retinopathy, can lead to tractional retinal detachment. In advanced cases, abnormal blood vessels and scar tissue form on the retina, pulling it away from the back of the eye. This type of retinal detachment progresses gradually and may cause distorted vision, dark shadows, or central vision loss. Managing blood sugar levels and undergoing regular diabetic eye screenings can help prevent retinal separation.
What are the Risk Factors of Retinal Detachment?
Here are some of the many risk factors of retinal detachment:
Several risk factors increase the likelihood of developing retinal detachment. While some people may have a genetic predisposition, others may develop it due to injuries or underlying conditions. Below are the key risk factors:
• History of Retinal Detachment in One Eye
People who have had retinal detachment in one eye are at a higher risk of developing it in the other eye. Regular monitoring and timely intervention can help prevent further complications.
• History of Eye Surgeries (e.g., Cataract Removal)
Individuals who have undergone cataract surgery or other intraocular procedures are more susceptible to retinal detachment. Surgical interventions can sometimes lead to vitreous detachment, increasing the chances of a retinal tear.
• Aging as a Risk Factor
Age-related changes in the vitreous gel inside the eye can contribute to retinal separation. As people age, the vitreous shrinks and may pull away from the retina, causing tears that lead to detachment. The risk is significantly higher after the age of 50.
• Severe Eye Injury and Retinal Detachment
Blunt trauma or penetrating injuries to the eye can cause retinal detachment by tearing the retina. Individuals involved in contact sports, high-impact activities, or accidents should take precautions to protect their eyes.
• Family History of Retinal Detachment
Genetics play a role in retinal detachment causes. If a close family member has experienced retinal detachment, the likelihood of developing the condition is higher. Routine eye checkups are essential for early detection.
• Myopia (Nearsightedness) and Retinal Detachment
People with high myopia (extreme nearsightedness) have elongated eyeballs, which stretch and thin the retina. This makes them more prone to lattice retinal degeneration and spontaneous retinal detachment.
• Underlying Eye Disorders and Diseases
Individuals with pre-existing eye conditions such as uveitis, lattice degeneration, retinoschisis, or Coats’ disease are at greater risk of retinal detachment. These diseases weaken retinal structures, making them more vulnerable to separation.
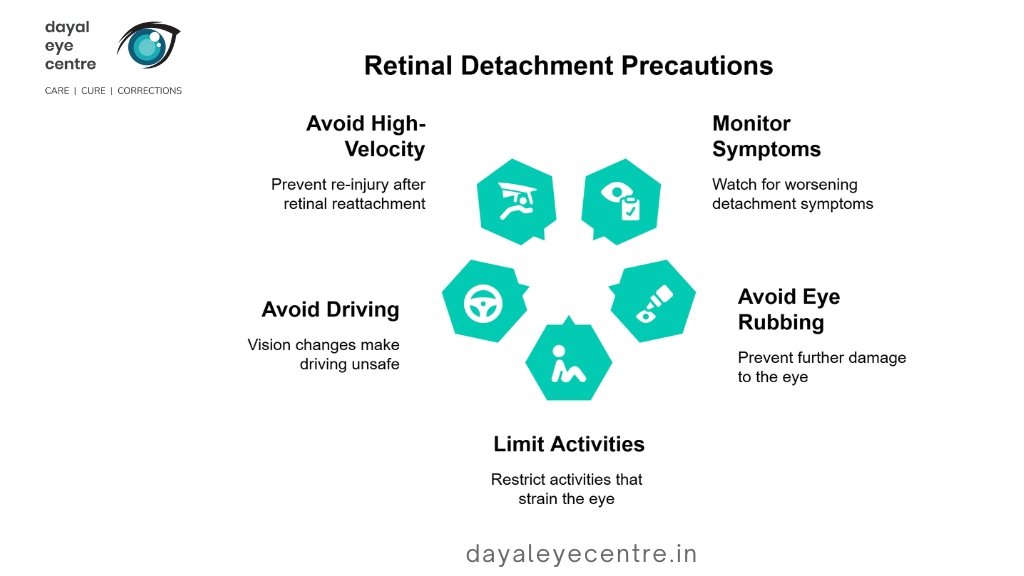
Retinal Detachment Prevention
Preventing retinal detachment is crucial, especially for individuals at higher risk due to factors like myopia, previous eye surgeries, or systemic conditions like diabetes. While not all cases of retinal separation can be avoided, the following preventive measures can help reduce the risk:
Avoid Direct and Indirect Eye Injuries
Eye trauma is a significant cause of retinal detachment, especially in people engaged in contact sports, hazardous jobs, or high-impact activities. To minimize the risk:
• Wear protective eyewear while playing sports like boxing, basketball, or racquetball.
• Use safety goggles when working in environments with flying debris or chemicals.
• Avoid rubbing the eyes aggressively, as excessive force can strain the retina.
• After an eye injury, seek immediate medical evaluation to rule out retinal tears or detachment.
Regular Eye Checkups
Routine eye examinations are vital for detecting early signs of retinal detachment, especially in individuals with high myopia, family history of retinal detachment, or pre-existing retinal conditions like lattice degeneration.
• People over 40 or those with risk factors should have an annual dilated eye exam.
• If experiencing retinal detachment eye flashes, sudden floaters, or vision distortions, consult an ophthalmologist immediately.
• Retinal detachment vision simulator tests can help patients understand potential vision changes and take preventive action.
Controlling Systemic Risk Factors and Diseases (e.g., Diabetes) Systemic conditions such as diabetes and high blood pressure increase the likelihood of tractional retinal detachment due to abnormal blood vessel growth. To minimize risk:
• Maintain optimal blood sugar levels to prevent diabetic retinopathy.
• Manage high blood pressure and cholesterol through lifestyle modifications.
• Follow a healthy diet rich in antioxidants and omega-3 fatty acids, which support retinal health.
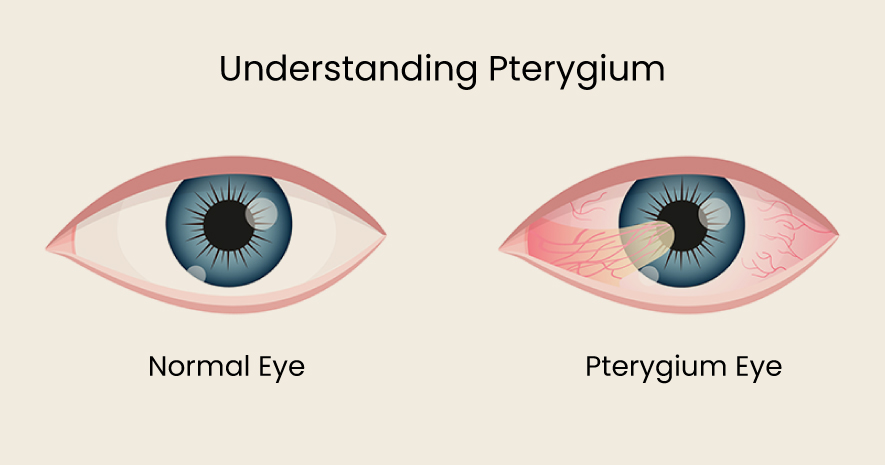
- What is Pterygium (Surfer’s Eye)?
Pterygium, commonly known as Surfer’s Eye, is a non-cancerous growth of tissue on the white part of the eye (conjunctiva) that can extend onto the cornea. It often develops in individuals frequently exposed to UV rays, wind, and dust—hence the name “Surfer’s Eye.” This condition can cause discomfort, vision disturbances, and, in severe cases, interfere with eyesight.
Although pterygium is not life-threatening, it can be progressive, requiring medical intervention in some cases. Early detection and management can prevent complications, making awareness essential for individuals at risk.
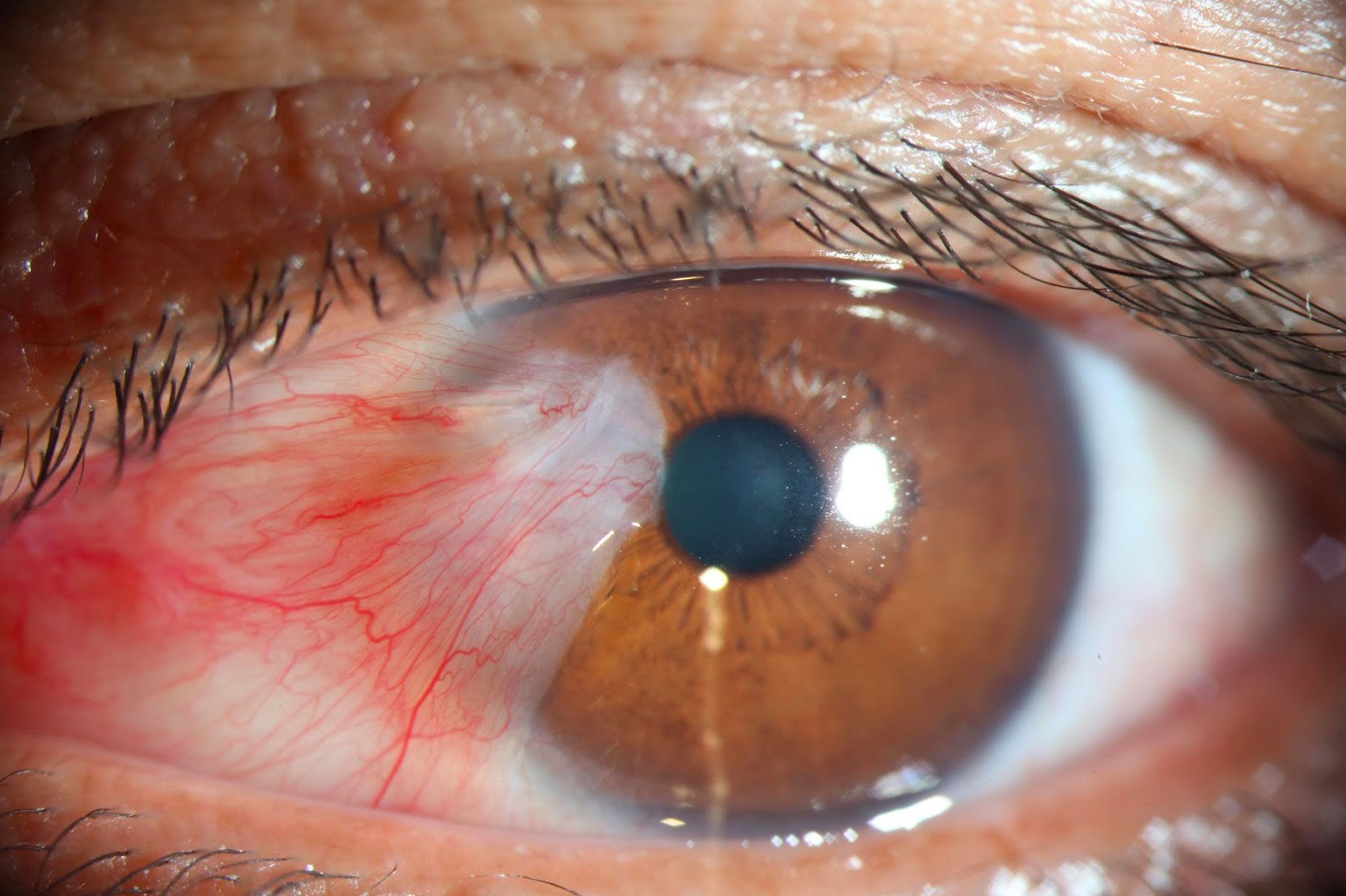
Symptoms of Pterygium (Surfer’s Eye)
Pterygium symptoms vary depending on its size, growth rate, and location. Common signs include:
• Foreign Body Sensation
A persistent feeling of something stuck in the eye is common, leading to discomfort, excessive blinking, or rubbing.
• Tearing from the Eyes
Excessive tearing, also called epiphora, occurs as the eye tries to remove irritation caused by the growth.
• Dryness of the Eyes
Pterygium disrupts the normal tear film, leading to chronic dry eyes, discomfort, and irritation.
• Redness
Due to inflammation, the affected eye often appears red and irritated, especially after exposure to wind or sunlight.
• Blurred Vision
As the pterygium extends onto the cornea, it can distort vision, leading to blurred or obstructed eyesight.
• Eye Irritation
A growing pterygium can cause itching, burning, and overall discomfort, especially in dry or dusty environments.
Causes of Pterygium (Surfer’s Eye)
Pterygium is strongly linked to environmental factors, especially exposure to UV rays, wind, and dust. Other contributing factors include:
• UV Exposure (Biggest Risk Factor)
Prolonged exposure to ultraviolet (UV) radiation from the sun is the primary cause of pterygium. This explains why it is commonly seen in surfers, fishermen, and outdoor workers.
• Chronic Eye Irritation
Frequent exposure to dry, dusty, or smoky environments increases irritation, making individuals more susceptible to pterygium.
• Wind and Sand Exposure
High-wind environments, especially in coastal areas, can lead to increased evaporation of tears, making the eyes dry and prone to irritation.
• Genetic Factors
Studies suggest that genetics may play a role in pterygium development, with some individuals being more prone to the condition.
• Contact Lens Use & Eye Strain
Excessive contact lens wear or digital eye strain may contribute to discomfort and increase the risk of pterygium self-care negligence.
Prevention Tips: How to Reduce the Risk of Pterygium?
• Wear UV-Protective Sunglasses– Reduces UV exposure
• Use Lubricating Eye Drops– Prevents dryness and irritation
• Limit Outdoor Exposure– Avoid peak sun hours (10 a.m. – 4 p.m.)
• Wear Hats & Protective Eyewear– Acts as an extra barrier
• Stay Hydrated– Keeps eyes moist and reduces irritation
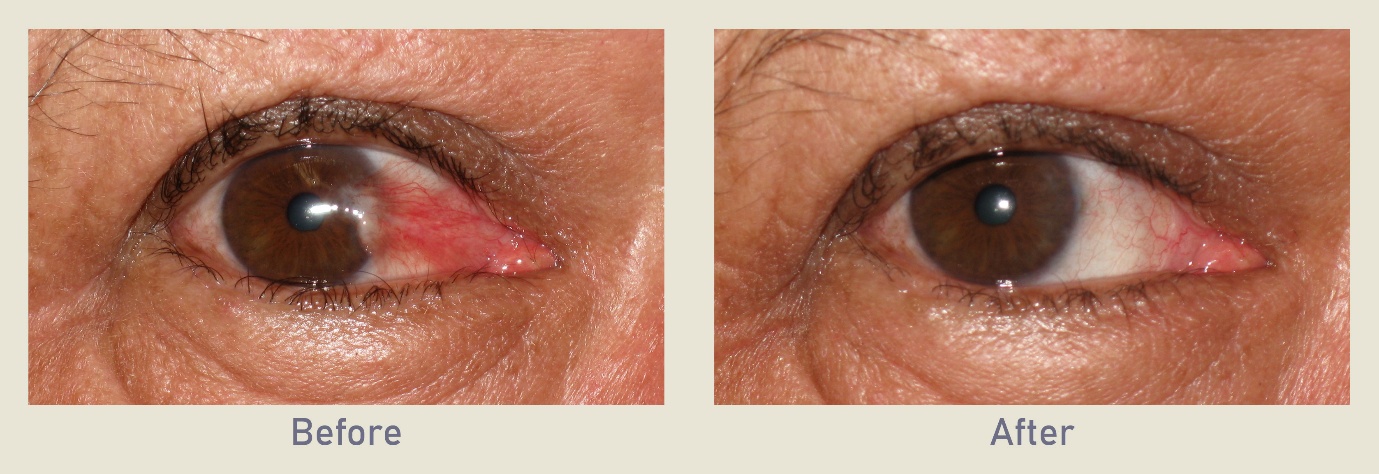
- What is Uveitis Eye?
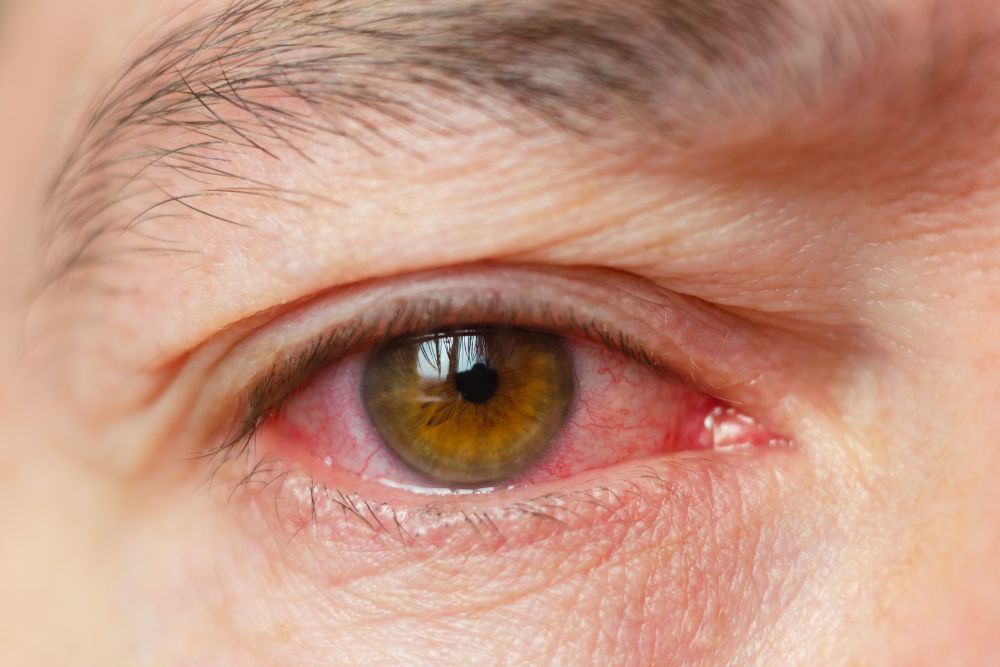
The uvea is the middle layer of the eye which contains much of the eye’s blood vessels. It is located between the sclera, the eye’s white outer coat, and the inner layer of the eye called the retina and is further made up of the iris, ciliary body, and choroid.
Uveitis encompasses a group of inflammatory diseases that produces swelling of the uveal tissues. It is not necessarily limited to the uvea but can also affect the lens, retina, optic nerve, and vitreous, producing reduced vision or blindness.
Uveitis may be caused by problems or diseases occurring in the eye, or it can be part of an inflammatory disease affecting other parts of the body.
It can happen at all ages and primarily affects people between 20-60 years old. Uveitis can last for a short (acute) or a long (chronic) time. The severest forms of uveitis can reoccur many times.
What are the Symptoms of Uveitis Eye?
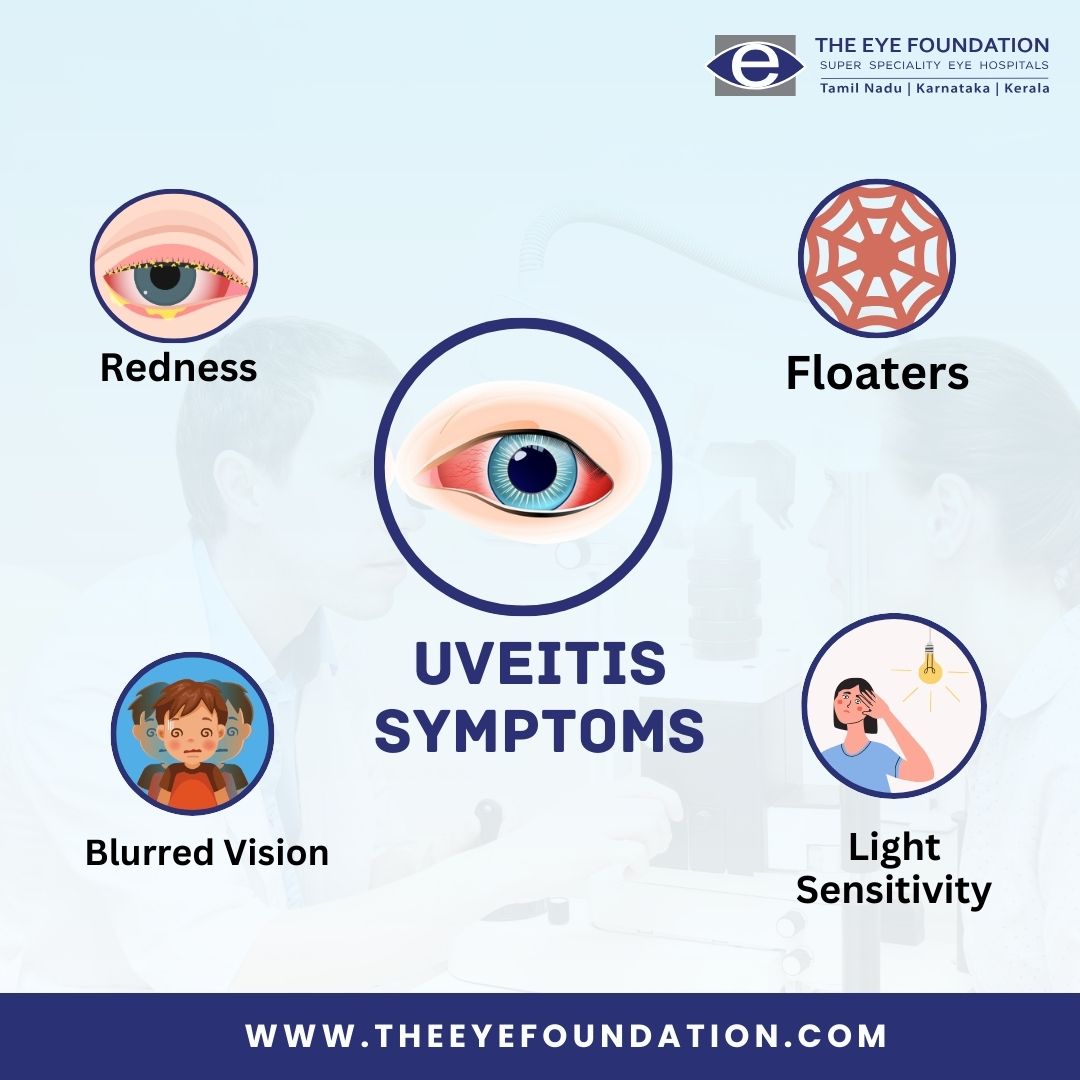
Uveitis can affect one or both eyes simultaneously. Symptoms may develop rapidly and can include:
• Blurred vision
• Dark, floating spots/lines in the vision (floaters)
• Eye pain
• Redness of the eye
• Sensitivity to light (photophobia)
The signs and symptoms of uveitis depend on the type of inflammation. Acute anterior uveitis may occur in one or both eyes and in adults is characterized by eye pain, blurred vision, sensitivity to light and redness. Intermediate uveitis causes blurred vision and floaters. Usually, it is not associated with pain.
Posterior uveitis can produce vision loss. This type of uveitis can only be detected during an eye examination.
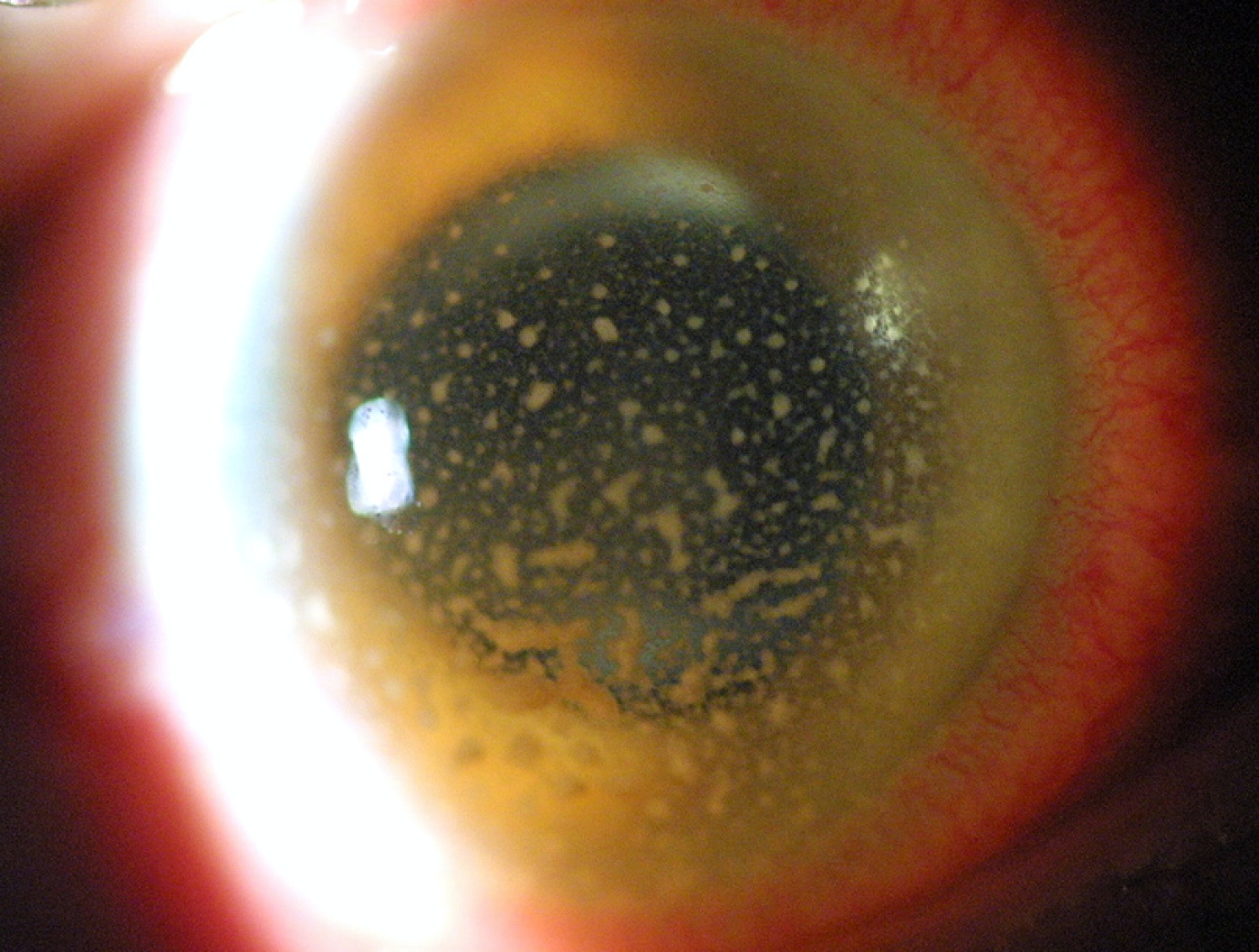
What are the Causes of Uveitis Eye?
Inflammation is the body’s natural response to tissue damage, germs, or toxins. It produces swelling, redness, and heat and destroys tissues as certain white blood cells rush to the affected part of the body to contain or eliminate the insult. Any inflammation of the uveal tissue produces Uveitis.
Uveitis may be caused by:
• An attack from the body’s own immune system (autoimmunity)
• Infections or tumors occurring within the eye or in other parts of the body
• Trauma to the eye
• Drugs and toxins
• Most of the times the cause remains unknown which is termed as idiopathic
What are the complications of Uveitis?
Many cases of uveitis are chronic, and they can produce numerous possible complications, including clouding of the cornea, cataracts, elevated eye pressure (IOP), glaucoma, swelling of the retina or retinal detachment. These complications can result in permanent vision loss.

If you Have Any Questions Call Us On +91 8985657102
Get an Appointment
Please fill in the form below!
Appointment TIMINGS are 9.30am TO 1.30pm ONLY
- What is Blepharitis (Eyelid Inflammation)?
